- Module 2 Overview
Self-Study Lessons - 0%Lesson 1
Chlamydial InfectionsActivities- 0%Lesson 2
Gonococcal InfectionsActivities- 0%Lesson 3
SyphilisActivities- 0%Lesson 4
Syphilis During Pregnancy and Congenital SyphilisActivities- 0%Lesson 5
Genital HerpesActivities- 0%Lesson 6
Human Papillomavirus InfectionActivities- 0%Lesson 7
Pelvic Inflammatory DiseaseActivities- 0%Lesson 8
VaginitisActivities- 0%Lesson 9
MpoxActivities- 0%Lesson 10
Mycoplasma genitaliumActivitiesLesson 4. Syphilis During Pregnancy and Congenital Syphilis
PDF ShareLast Updated: August 25th, 2025Authors:David H. Spach, MD,David H. Spach, MD
Editor-in-Chief
Professor of Medicine
Division of Allergy and Infectious Diseases
University of WashingtonDisclosures: NoneEmily H. Adhikari, MD,Emily H. Adhikari, MD
Assistant Professor, Department of Obstetrics and Gynecology
UT Southwestern Medical Center
Medical Director of Perinatal Infectious Diseases
Parkland Health and Hospital SystemJason E. Zucker, MDJason E. Zucker, MD
Assistant Professor of Medicine
Columbia University Irving Medical Center
Assistant Medical Director
New York City STD Prevention Training CenterDisclosures: NoneLearning Objective Performance Indicators
- Summarize epidemiologic trends in syphilis in pregnancy and congenital syphilis
- Routinely screen all pregnant women for syphilis
- Administer recommended treatment for pregnant women diagnosed with syphilis
- Select appropriate treatment for congenital syphilis when indicated
- Provide recommended evaluation and monitoring of neonates born to mothers with syphilis
Table of Contents- Syphilis During Pregnancy and Congenital Syphilis
- Welcome Video
- Introduction
- Epidemiology in the United States
- Pathogenesis and Transmission
- Clinical Manifestations of Syphilis in Women
- Laboratory Tests Used for Syphilis Screening and Diagnosis
- Screening Recommendations for Pregnant Women
- Evaluation and Diagnosis of Intrauterine Fetal Syphilis Infection
- Treatment of Syphilis During Pregnancy
- Treatment of Primary and Secondary Syphilis in Pregnancy
- Treatment of Latent Syphilis During Pregnancy
- Treatment of Neurosyphilis, Ocular Syphilis, or Otosyphilis During Pregnancy
- Treatment of Tertiary Syphilis During Pregnancy
- Management of Pregnant Women Exposed to a Sex Partner with Syphilis
- Treatment of Syphilis in Pregnancy in Persons Allergic to Penicillin
- Jarisch-Herxheimer Reaction in Pregnancy
- Efficacy of Syphilis Treatment During Pregnancy
- Follow-Up of Women Treated for Syphilis During Pregnancy
- Clinical Manifestations of Syphilis in Neonates and Young Children
- Screening and Evaluation of Syphilis in Neonates
- Management of Neonates and Young Children Born to Mothers Diagnosed with Syphilis
- Antimicrobial Therapy for Treating Congenital Syphilis
- Evaluation of Neonates Born to Mothers Diagnosed with Syphilis During Pregnancy
- Category 1: Confirmed Proven or Highly Probable Congenital Syphilis
- Category 2: Possible Congenital Syphilis
- Category 3: Congenital Syphilis Less Likely
- Category 4: Congenital Syphilis Unlikely
- Additional Scenarios Related to Maternal Syphilis Serologic Testing
- Treatment of Infants and Children Older than 1 Month of Age
- Follow-Up of Neonates and Infants
- Summary Points
- Check-On-Learning
- Citations
- Additional References
- Figures
- Tables
Welcome Video
Activity: Welcome VideoInstructions: Watch the brief welcome video by Dr. Cynthia Gyamfi-Bannerman (1 minute and 30 seconds)Introduction
Congenital syphilis is defined as the transmission of the spirochete bacterium, Treponema pallidum, from a mother to her fetus or infant. In utero fetal infection, especially when maternal syphilis is not treated early in pregnancy, can result in severe adverse outcomes, including stillbirth, hydrops fetalis, as well as neonatal and childhood complications.[1,2,3] Congenital syphilis is a preventable disease. Effective prevention depends on consistent screening for syphilis during pregnancy, prompt maternal syphilis treatment with penicillin, evaluation of the neonate at birth for possible syphilis treatment, and appropriate follow-up of the mother and infant. Tragically, in recent years in the United States, more than 80% of cases of congenital syphilis occur in mothers who were either not screened on a timely basis during pregnancy or were not appropriately treated if diagnosed with syphilis.[4,5] Efforts to address and prevent congenital syphilis need to involve all health care team members who may potentially have an encounter with a pregnant woman, including obstetricians, midwives, family medicine physicians who include obstetrics in their practice, nurses, advanced practice providers, maternal fetal medicine specialists, emergency room clinicians, pediatricians, neonatologists, and infectious diseases specialists. In addition, congenital syphilis prevention efforts need to span all high-impact potential points of intervention, including prepregnancy, during pregnancy, at birth, and in the neonatal period (Figure 1).[6] This lesson will focus on the comprehensive aspects of maternal syphilis and congenital syphilis. For more details about syphilis in general, see the Syphilis Lesson on this site.
Epidemiology in the United States
To better understand the impact and trends of congenital syphilis in the United States, it is important to understand (1) the epidemiology of syphilis in women of childbearing age, including syphilis cases in pregnant women, and (2) the epidemiology of congenital syphilis cases.[4]
Cases of Syphilis in Women of ChildBearing Age
In 2023, there were 54,932 reported cases of Syphilis (all stages) among women 15–44 years of age. In the United States, the highest number of reported cases of syphilis in women 15–44 years of age were from Texas (7,993 cases) and California (7,519 cases).[4] Reported cases of syphilis (all stages) in pregnant women increased steadily from 2018 to 2023.[4] Since women are most likely to transmit syphilis to the fetus during early syphilis, cases of primary and secondary syphilis have particular importance. The rate of primary and secondary syphilis among women 15–44 years of age has increased more than 8-fold since 2014.[4] In 2023, the rate of primary and secondary syphilis in women 15–44 years of age was highest in women in the 25–29 years of age (Figure 2).[4]
Cases of Congenital Syphilis
In 2023, there were 3,882 cases of congenital syphilis reported in the United States, which included a total of 252 congenital syphilis-related stillbirths and 27 infant deaths.[4] In 2023, the rate of congenital syphilis cases was 105.8 per 100,000 live births. In the past 10 years, the number of reported cases of congenital syphilis has increased more than 8-fold.[4] The increase over the past 10 years slowed recently, with an increase of only 3% from 2022 to 2023.[4] The number of cases of congenital syphilis was highest with Hispanic/Latino, Black, and White birth parents; the rates were highest with American Indian/Alaska Native birth parents.[4] The increased rate of reported cases of congenital syphilis parallels the overall increase in syphilis cases in women of childbearing age (Figure 3).[4]
Outcomes of Congenital Syphilis Births
In the United States in 2023, among the 3,882 cases of congenital syphilis, the birth outcomes were as follows: 252 (6.5%) stillbirths, 27 cases (0.7%) of neonatal/infant deaths, 1,295 (33.4%) were born alive with congenital syphilis-related signs or symptoms, 2,282 cases (58.8%) were born alive with no documented congenital syphilis-related signs or symptoms, and 26 (0.7%) were missing information on vital status (Figure 4).[4]
Pathogenesis and Transmission
Congenital syphilis results from the transmission of T. pallidum from a mother to a child during pregnancy, or less often, at the time of delivery. The in-utero transmission typically occurs during maternal disseminated bloodstream infection, which results in invasion of the placenta by T. pallidum, followed by transmission across the placental barrier.[7,8] Usually, the placenta keeps the maternal and fetal compartments separate, but T. pallidum overcomes this barrier through unknown mechanisms.[8,9,10] Once across the placental barrier, T. pallidum flows into the umbilical vein, which is followed by a hematogenous systemic infection in the fetus; the limited outer membrane protein expression of T. pallidum helps it evade the fetal immune system and thereby cause persistent infection in the fetus.[9,11,12,13] After placental infection occurs, T. pallidum is consistently present in amniotic fluid.[3,14] Occasional cases of congenital syphilis and T. pallidum transmission have occurred at birth from newborn contact with maternal blood, secretions, or genital lesions.[8,11,12] Transmission of T. pallidum is not known to occur via breastmilk, but transmission can theoretically occur during breastfeeding if the mother has primary or secondary syphilitic lesions on her breast.[12] When considering the pathogenesis of congenital syphilis, it is important to consider the factors related to the risk of transmission and those factors that can influence the outcome of the infection in the child. These outcomes include stillbirth, hydrops fetalis, asymptomatic infection, early congenital syphilis, and late congenital syphilis.
Relative Risk of Transmission
The relative risk of in utero transmission of T. pallidum from mother to fetus strongly correlates with the stage of maternal syphilis, with transmission most likely to occur with early syphilis infection, particularly during the secondary syphilis stage when disseminated bloodstream infection occurs (Figure 5).[12] Available data suggest mothers with untreated early syphilis (infection for less than 1 year) have a rate of transmission to the fetus of approximately 50-70%, whereas with untreated late syphilis infection (infection more than 1 year prior), this risk decreases to approximately 10-15%.[3,7,15,16] Transmission of T. pallidum to the fetus can occur at any time in the pregnancy (in any trimester), and the previous hypothesis that T. pallidum could not penetrate the placenta prior to gestation week 20 has been disproven.[8] The risk of transmission is also impacted by the timeliness and effectiveness of treatment. Immediate and effective treatment of the mother when diagnosed with syphilis, especially with early syphilis, will markedly reduce the risk of transmission to the fetus.
Outcome of Fetal Infection
The clinical outcome of untreated fetal T. pallidum infection is influenced by the timing of vertical transmission during pregnancy. Transmission occurring in the first or second trimester, particularly in the absence of maternal treatment, carries a higher risk of causing congenital syphilis.[7] The risk of congenital syphilis is greatest when conception occurs during untreated primary or secondary syphilis.[7,15] In contrast, fetal T. pallidum infection later in pregnancy is generally associated with more favorable outcomes. By the third trimester, fetal organogenesis is largely complete, and the immunologic environment of the fetoplacental unit tends to promote fetal preservation.[7] Neonates infected in the third trimester are more likely to be asymptomatic at birth, but in the absence of treatment, clinical manifestations of congenital syphilis may emerge postnatally.[3,7,15] There is also evidence for an increased incidence of fetal demise very shortly after acute T. pallidum infection, potentially mediated by a robust maternal or fetal inflammatory response characterized by elevated cytokine release.[7] The prognosis for the fetus is further shaped by the timing and adequacy of antimicrobial therapy for syphilis. In general, a prolonged duration of untreated maternal infection correlates with poorer neonatal outcomes. It is important to note that even with appropriate antimicrobial treatment, the risk of congenital syphilis is not entirely eliminated.
Clinical Manifestations of Syphilis in Women
Natural History of Syphilis Infection in Women
Women who develop congenital syphilis can acquire T. pallidum prior to pregnancy or during pregnancy. The natural history of syphilis in women is not significantly altered by pregnancy.[3,16] Exposure to and acquisition of T. pallidum is typically followed by an incubation period of 10–90 days before the first clinical manifestation becomes evident.[17] Syphilis is conceptually thought of as occurring in stages, including primary, secondary, latent, and tertiary; the staging of syphilis is also conceptually divided into early and late syphilis (Figure 6). Typically, early syphilis refers to the first year of T. pallidum infection and includes primary, secondary, and early latent (asymptomatic) syphilis.[3,18,19] Late syphilis results from untreated (or inadequately treated) syphilis and includes late latent and tertiary syphilis. Neurologic syphilis, ocular syphilis, and otosyphilis can occur early or late in the course of syphilis.
Clinical Presentation of Syphilis in Women
The clinical manifestations of syphilis in women are not significantly altered by pregnancy.[3,16] It is important to recognize syphilis-related clinical manifestations in pregnant women and in women of childbearing age who may become pregnant. Because transmission is most likely to occur with early syphilis, it is extremely important that clinicians can recognize manifestations of primary and secondary syphilis in women.
Primary Syphilis
Following the inoculation of T. pallidum at a mucocutaneous entry site, organisms proliferate, sensitize lymphocytes, and activate macrophages, causing the formation of a primary lesion or “chancre” in the area of the inoculation. In women, primary syphilis most often manifests as a painless, solitary oral or labial lesion that can develop either on the external skin or internally on the mucosal surface (Figure 7). Regional firm lymphadenopathy frequently develops in proximity to the primary lesion. Less often, primary syphilis in women manifests in the anal or perianal region. Syphilitic chancres typically progress from a papule to a painless ulcer that is usually well-circumscribed, with a clean base and heaped-up margins. Less often, women with primary syphilis can develop multiple or painful lesions.
Secondary Syphilis
Secondary lesions reflect hematogenous dissemination of T. pallidum and generally appear 4 to 10 weeks after the onset of the primary chancre.[17] In fewer than 10% of cases, primary and secondary stages may overlap.[20] Signs and symptoms of secondary syphilis are often the first observed clinical manifestation of syphilis, as primary lesions are often overlooked or not recognized.[20] Relapses of secondary symptoms occur in up to 25% of untreated persons. A wide array of manifestations can occur with secondary syphilis in women (Figure 8).[3,16,21]
- Generalized Body Rash: The rash that occurs in secondary syphilis is typically a diffuse, nonpruritic rash that characteristically involves the chest, back, palms, and soles. The skin lesions are typically 1 to 2 cm in size and can appear as any combination of macular, papular, squamous, or pustular forms. In lighter-skinned women, the skin lesions are usually red or copper-colored, but in darker-skinned women, they may also appear as brown or hyperpigmented lesions.
- Lymphadenopathy: Approximately 50 to 86% of persons with secondary syphilis develop lymphadenopathy, which may be diffuse.
- Systemic Symptoms: Patients often present with malaise, fever, and other nonspecific constitutional symptoms.
- Mucous Patches: The development of mucous patches occurs in 6 to 30% of patients and manifests as flat patches located in the oral cavity, pharynx, larynx, or genital region.
- Condylomata Lata: Approximately 10 to 20% of persons with secondary syphilis will have condylomata lata lesions, which appear as moist, heaped-up, wart-like papules in warm, intertriginous areas (most commonly gluteal folds, perineum, and perianal); these lesions are highly contagious.
- Alopecia: About 5% of patients develop patchy alopecia, most often in the occipital or bitemporal scalp region, but some patients will have loss of the lateral region of the eyebrows.
- Visceral Organ Involvement: In some cases, syphilis may involve one or more visceral organs, including the liver, kidney, lungs, gastrointestinal tract, and spleen. The most common visceral organ manifestations are nephritis and hepatitis (with a high alkaline phosphatase level).
Latent Infection
Latent syphilis describes the diagnosis of syphilis based on syphilis serologic screening results in a person who does not have current or recent syphilis-related manifestations. Women diagnosed with syphilis in pregnancy most often have this occur through routine screening. Most women diagnosed with syphilis in pregnancy do not have any syphilis-related clinical manifestations, so they are diagnosed with latent syphilis. Latent syphilis is classified into early latent and late latent.[19] Understanding how to categorize syphilis into early latent and late latent is important, since transmission of T. pallidum is more likely with early infection, and management differs with early and late latent syphilis.[11,12,19]
- Early Latent Syphilis (Infection of Less than 1 Year in Duration): Persons with latent syphilis are classified in the subcategory of early latent syphilis if they have no clinical signs or symptoms of syphilis and ANY of the following:[19]
- A documented seroconversion within the previous 12 months
- A documented sustained (greater than 2 weeks) fourfold or greater increase in a nontreponemal test titer during the 12 months preceding the diagnosis in a person previously treated for syphilis
- Unequivocal symptoms of primary or secondary syphilis within the prior 12 months
- Contact in the prior 12 months with a sex partner who had untreated primary, secondary, or early latent syphilis
- Documented reactive nontreponemal and treponemal tests, and the only possible exposure occurred during the previous 12 months
- Late Latent or Latent Unknown Duration Syphilis (Infection Greater than 1 Year in Duration): Persons are considered to have late latent syphilis (or syphilis of unknown duration) if they meet ALL the following criteria:[19]
- A reactive nontreponemal and treponemal test
- No clinical manifestations of syphilis
- Does not meet any of the criteria for early latent syphilis
Tertiary Syphilis
In the modern era, a diagnosis of tertiary syphilis is rare, especially in younger women of childbearing age. Tertiary syphilis can develop 2–30 years after initial acquisition of T. pallidum and can manifest as gummatous disease, cardiovascular syphilis, late neurosyphilis, late ocular syphilis, or late otic syphilis. Expert consultation is advised if tertiary syphilis is diagnosed (or strongly suspected). Women with tertiary syphilis, including pregnant women, have an extremely low risk or no risk of transmitting T. pallidum to others or to their fetus, but require treatment to reduce the complications of tertiary syphilis.
Neurosyphilis
Neurologic manifestations caused by syphilis can occur early or late in the course of the infection.[17,18] Making a diagnosis of neurosyphilis includes a combination of clinical findings, reactive syphilis serologic studies, and characteristic abnormalities detected on cerebrospinal fluid (CSF) analysis. Common neurologic manifestations include severe headache or meningitis, cranial nerve palsies, stroke, or cognitive dysfunction. Making a diagnosis of neurosyphilis is extremely important since management requires intravenous treatment.[19]
Ocular Syphilis
Ocular manifestations caused by syphilis can also occur early or late in the course of the infection.[17,18] Syphilis-related ocular abnormalities can involve any part of the eye.[22,23] Making a diagnosis of ocular syphilis requires a combination of ocular symptoms, abnormal ocular findings confirmed by an ophthalmologist, and reactive syphilis serologic studies. Uveitis is the most common ocular abnormality, and this may manifest as anterior, posterior, or panuveitis.[22,23] Any woman with a suspected diagnosis of ocular syphilis should have a neurologic examination and prompt referral made to an ophthalmologist. Making a diagnosis of ocular syphilis is extremely important since rapid permanent loss of visual function can occur, and management requires intravenous treatment.[19]
Otosyphilis
Otosyphilis, similar to neurosyphilis and ocular syphilis, can occur early or late in the course of the infection.[17,18] Common syphilis-related otic abnormalities include hearing loss, tinnitus, vertigo, or a combination of these manifestations.[24,25] Otic manifestations can be unilateral or bilateral.[24,25] Any woman with a suspected diagnosis of otosyphilis should have a neurologic evaluation and receive a prompt referral for an auditory examination by an otolaryngologist or audiologist. Making a diagnosis of neurosyphilis is extremely important since rapid permanent loss of hearing can occur, and management requires intravenous treatment.[19]
Laboratory Tests Used for Syphilis Screening and Diagnosis
Serologic testing for syphilis involves the use of both treponemal (antibody) and nontreponemal (lipoidal antigen) tests.[26] Making a serologic diagnosis of syphilis requires reactive tests with both treponemal and nontreponemal serologic tests. The following summarizes basic information about the serologic tests used to diagnose syphilis. Screening recommendations and algorithms are discussed in the sections on Screening Recommendations for Pregnant Women and Screening and Evaluation of Syphilis in Neonates and Young Children. The major limitation of treponemal tests is the inability to distinguish between recent and prior infections, since most persons with a prior history of syphilis maintain a positive treponemal (antibody) test for life. Therefore, individuals with a prior history of syphilis usually require rescreening using a nontreponemal test (Venereal Disease Research Laboratory [VDRL] or rapid plasma reagin [RPR]).[26] In addition, false-negative syphilis serologic tests can occur among persons with primary syphilis due to absent or very low levels of antitreponemal antibodies very early after infection.[26]
Types of Syphilis Serologic Tests
- Treponemal Serologic Tests (EIA, CIA, TP-PA, FTA-ABS): The laboratory-based treponemal serologic tests include enzyme immunoassays (EIA), chemiluminescence immunoassay (CIA), T. pallidum particle agglutination (TP-PA), and fluorescent treponemal antibody absorption (FTA-ABS) tests. These tests directly measure antibodies targeted against T. pallidum antigens and provide a qualitative test result. Direct treponemal tests usually become reactive earlier than with nontreponemal tests after T. pallidum infection. For initial screening, the automated EIA or CIA test is usually used. When further testing of discordant initial treponemal and non-treponemal test results is needed, an additional and different treponemal test (TP-PA or FTA-ABS) is used.[26] Nearly all persons diagnosed with syphilis will maintain a reactive treponemal test for life, except for some persons treated during the primary stage of syphilis, who eventually revert to being serologically nonreactive. Thus, the major limitation of treponemal tests is the inability to distinguish between current, recent, and past infection.
- Nontreponemal Serologic Tests (RPR, VDRL): The commonly used nontreponemal tests are the rapid plasma reagin (RPR) and the Venereal Disease Research Laboratory (VDRL) tests.[26] These tests are often referred to as “lipoidal antigen” tests since they measure antibodies directed against lipoidal antigens, such as cardiolipin and lecithin, which are released from damaged host cell membranes and T. pallidum membranes.[26,27] When an RPR or VDRL test is reactive, the laboratory typically follows this with a quantitative RPR or VDRL titer. The RPR and VDRL titers correlate with disease activity, and a fourfold or greater change in titer (e.g., from 1:16 to 1:4 or from 1:8 to 1:32) is considered evidence of a clinically significant difference.[26] Nontreponemal tests are labor-intensive to perform, and biologic false-positive tests can occur. When comparing sequential test results, such as during follow-up or between neonatal and maternal titers, the same test method (either VDRL or RPR) should be used to ensure consistency.
- Point-of-Care Tests for Syphilis: There are two point-of-care tests authorized by the United States Food and Drug Administration (FDA) for point-of-care syphilis testing: (1) Syphilis Health Check Treponemal Antibody Test (SHC) and (2) ChemBio DPP HIV-Syphilis (ChemBio DPP), which detects HIV as well as syphilis.[28] Both assays typically use whole blood collected from a fingerstick and require approximately 15 minutes to perform.[28] These tests are treponemal (antibody) tests and have a lower sensitivity and specificity than laboratory-based treponemal tests.[28] To make a serologic diagnosis of syphilis, a positive point-of-care test result must be confirmed by a laboratory-based serologic test and a second treponemal (antibody) test.[28] In addition, if there is a high index of suspicion for a diagnosis of syphilis and the point-of-care syphilis test is negative, further testing with a laboratory-based syphilis test should be performed.
Syphilis Serologic Testing in Pregnancy
Available data suggest that pregnancy does not significantly alter the sensitivity and specificity of treponemal (antibody) and nontreponemal (lipoidal antigen) serologic tests.[26,29,30] Performing routine universal screening for syphilis in pregnant women will result in screening a population with a lower prevalence of syphilis than if performing targeted screening of populations at risk for syphilis. Therefore, routine syphilis screening of pregnant women is associated with more false-positive and discordant results, especially when using treponemal antibody tests (EIA or CIA) as the initial screening test.[31] Recommendations advise that syphilis serologic test results should be interpreted the same way regardless of pregnancy status, but clinicians should be aware that in generalized screening of low-prevalence populations, such as all pregnant women, additional evaluation may be needed to resolve discordant test results.[26]
Syphilis Serologic Testing in Neonates
The diagnosis of congenital syphilis is often difficult since maternal nontreponemal and treponemal IgG antibodies can be transferred through the placenta to the fetus, and treponemal antibodies can persist for 15 months or longer.[19] The use of treponemal tests for neonates is not recommended due to the transfer of maternal antibodies. In addition, testing of umbilical cord blood is not recommended since it may become contaminated with maternal blood.[26] Serologic testing of neonates should utilize nontreponemal testing of neonatal serum; the type of nontreponemal test should be the same as the comparison test obtained at birth from the mother.[26] Evaluation and treatment of congenital syphilis is complex and should ideally include expert consultation.
Screening Recommendations for Pregnant Women
Routine screening for syphilis during pregnancy is of paramount importance in preventing congenital syphilis. In more than 80% of cases of congenital syphilis, the mother received no syphilis testing or inadequate syphilis testing.[5] The following summarizes syphilis screening recommendations for pregnant women, including the timing of screening and potential screening algorithms.
Syphilis Screening Recommendations for Routine Screening During Pregnancy
Routine screening for syphilis during pregnancy is critical in preventing congenital syphilis. In more than 80% of cases of congenital syphilis, the mother received no syphilis testing or inadequate syphilis testing.[5] All pregnant women should undergo screening for syphilis at the first care visit during pregnancy; this first care visit could occur at a prenatal visit, but could also occur at an urgent care visit, emergency room visit, etc. The rationale for routine syphilis screening at any health care encounter after known pregnancy is that approximately 40% of infants with congenital syphilis were born to women who had not received prenatal care. The following summarizes syphilis screening recommendations during pregnancy from the American College of Obstetrics and Gynecology (ACOG), CDC, Society for Maternal-Fetal Medicine (SMFM), and U.S. Preventive Services Task Force (USPSTF).
- ACOG: Perform syphilis serologic screening for all pregnant women at the first prenatal care visit, during the third trimester, and at birth.[32]
- CDC: Perform syphilis serologic screening for all pregnant women at the first health encounter during pregnancy. Screening at 28 weeks’ gestation and at delivery is recommended for women who (1) live in communities with high rates of syphilis, (2) are at high risk for syphilis acquisition during pregnancy because of geographical risk (counties in the United States with a rate of primary and secondary syphilis among women 15–44 years of age that is greater than 4.6 per 100,000 people [for county-specific information, see the Activity below]) or personal risk (e.g., substance use, sexually transmitted infection [STI] during pregnancy, multiple partners, a new sex partner, or partner with STI), or (3) were not previously tested during the pregnancy.[19,33] In addition, syphilis testing is recommended for any woman who has a fetal death after 20 weeks’ gestation. The CDC recommends that no mother or newborn infant should leave the hospital without maternal serologic status having been documented at least once during pregnancy.[19]
- SMFM: Perform syphilis serologic screening three times for all pregnant women: at initiation of prenatal care, during the third trimester, and at delivery. Pregnant women with a stillbirth and/or a fetus with nonimmune hydrops should have syphilis testing. All women diagnosed with syphilis during pregnancy should have HIV screening performed.
- USPSTF: Perform syphilis serologic screening for all pregnant women when they first present for care.[34] Screening for syphilis should occur as early in pregnancy as possible.[34] In addition, the USPSTF recommends that clinicians should be aware of the syphilis prevalence in their communities and be informed about their state mandate for syphilis screening.[34]
County-Level Rates of Primary and Secondary Syphilis Among Women Aged 15-44
The CDC has published United States county-based 2023 data on rates of primary and secondary syphilis among women who are 15–44 years of age.[35] Although these data are not taken from pregnant women, the information is highly relevant to congenital syphilis for two reasons: (1) these data capture the risk of syphilis for most women of childbearing age, and (2) the stages of syphilis reported (primary and secondary) are the stages associated with the highest risk for maternal-fetal transmission.
Activity: Explore County Syphilis RatesInstructions
Explore this interactive tool using either the interactive map or the drop-down menu. Note that with the interactive map, when you click on a state, the counties with rates above 4.6 per 100,000 women are yellow in color and those with rates at or below 4.6 per 100,000 women are green in color.Syphilis Screening Methods for Use During Pregnancy
The type of syphilis test used for initial screening depends on several factors, including whether the pregnant woman has previously received treatment for syphilis, the local laboratory or clinic protocol, state-required testing methods, and whether follow-up is uncertain. The three main types of screening algorithms are: (1) reverse screening, which uses initial testing with a laboratory-based treponemal test (CIA, EIA), (2) traditional screening algorithm, which uses initial testing with a laboratory-based nontreponemal test (RPR or VDRL); and (3) initial screening with a point-of care treponemal antibody test (EIA) (Figure 9).[26]
- Screening Women without Prior History of Syphilis: For routine screening in women who have never been diagnosed with syphilis, three main options exist for the initial syphilis serologic screening test: laboratory-based treponemal antibody tests (CIA, EIA), laboratory-based nontreponemal tests (RPR and VDRL), and the point-of-care treponemal antibody test.[26,28] When treponemal testing (CIA, EIA) is used as the initial screening test, this is referred to as the reverse screening algorithm. When a nontreponemal test (RPR or VDRL) is used as the initial screening, it is referred to as the traditional screening algorithm. The type of test initially used is often dictated by local laboratory, clinic, or hospital protocols. Point-of-care testing is most often used in situations where follow-up is uncertain, and an initial reactive test could be paired with same-day syphilis treatment. Regardless of which test is used, all initial reactive tests require follow-up confirmatory syphilis serologic testing with a different type of assay. Women without prior syphilis treatment who have a positive treponemal screening immunoassay, negative nontreponemal test, and positive second treponemal test should receive treatment for late latent syphilis, unless the history or examination indicates a recent exposure or other syphilis-related complications, such as neurologic involvement.
- Screening Women With a Prior History of Syphilis: For any pregnant woman who has previously been diagnosed with syphilis, nontreponemal assays (RPR or VDRL) should be used for syphilis serologic testing, since antibody-based treponemal tests (EIA and point-of-care tests) almost always remain positive for life after syphilis infection and thus cannot indicate when new infection has occurred.[26] When ordering and comparing nontreponemal tests, if possible, use the same type of test (VDRL or RPR). When interpreting nontreponemal tests in a person with a prior history of syphilis, a newly reactive nontreponemal test or a 4-fold increase in the titers (of the same type of test) is considered clinically significant and likely to represent a new T. pallidum infection.[19,26] It is important to emphasize that point-of-care treponemal testing is not recommended for persons with a prior history of syphilis.[26,28]Check-on-Learning QuestionWhich one of the following tests should ideally be ordered for the syphilis pregnancy screening test?Check
-On-
Learning
QuestionA 29-year-old woman is seen for her first prenatal visit, and she is about 15 weeks pregnant. She was diagnosed with secondary syphilis 1 year ago and received appropriate treatment. She has a pretreatment nontreponemal RPR titer of 1:128. Six months after treatment, the RPR titer had declined to 1:8. She has not had any additional follow-up syphilis serologic studies.Which one of the following tests should ideally be ordered for the syphilis pregnancy screening test?
Evaluation and Diagnosis of Intrauterine Fetal Syphilis Infection
All women diagnosed with syphilis during pregnancy should undergo evaluation for fetal T. pallidum infection. Potential strategies used to diagnose fetal infection with T. pallidum include (1) performing a fetal ultrasound to identify characteristic syphilis-related fetal abnormalities and infer the presence of congenital infection, or (2) obtaining fluid samples from amniocentesis for dark-field microscopy or nucleic acid amplification testing (NAAT) of amniotic fluid.[3,36] In most clinical settings, performing direct detection of T. pallidum in amniotic fluid is not available or practical. Therefore, fetal ultrasound is generally used as the method of choice for evaluating fetal syphilis.[3,16] Among pregnant women who acquire T. pallidum prior to pregnancy or early in pregnancy, abnormal fetal ultrasound findings do not usually become apparent until after gestation weeks 16-18, which corresponds to the time when the fetal immune system has sufficiently developed such that it can generate a robust inflammatory response to T. pallidum infection; it is the inflammatory response that causes the characteristic neonatal abnormalities.[3,36,37] Note that a normal fetal ultrasound does not exclude the diagnosis of congenital syphilis, since approximately 10% of neonates with congenital syphilis at birth have a normal antepartum pretreatment ultrasound (obtained prior to the mother receiving treatment for syphilis).[37]
- Recommendation: All women diagnosed with syphilis during pregnancy undergo fetal ultrasound after gestation week 18 to evaluate for fetal intrauterine infection. Although findings on fetal ultrasound will not change the maternal syphilis treatment regimen, the ultrasound provides insight into infants likely to need treatment for congenital syphilis, since women with an abnormal ultrasound are more likely to have treatment failure, have obstetric complications, and give birth to infants who require treatment for neonatal syphilis.[37] In addition, the initial ultrasound serves as a baseline for monitoring the response to treatment with fetal abnormalities if they are evident on the initial ultrasound.
- Follow-Up Ultrasound: The recommendations for scheduled follow-up fetal ultrasound testing should be considered in consultation with an expert, and follow-up ultrasound testing depends on (1) the week of gestation the ultrasound was obtained and (2) whether the initial ultrasound was abnormal.
Fetal Ultrasound Abnormalities
In a study that enrolled 235 pregnant women diagnosed with syphilis at week 18 gestation or later, fetal ultrasound was performed before syphilis treatment, and serial ultrasounds were performed after treatment.[37] Abnormal fetal ultrasound (at least 1 abnormality) was observed in 73 (31%) of the 235 pregnant women diagnosed with syphilis.[37] Among the 73 women with syphilis and abnormal fetal ultrasound findings, the most common abnormalities were hepatomegaly (79%), elevated peak systolic velocity of the middle cerebral artery (33%), which is a surrogate marker for neonatal anemia, placentomegaly (27%), polyhydramnios (12%); and ascites/nonimmune hydrops (10%).[37] Fetal hepatomegaly is thought to be multifactorial and caused by syphilitic hepatitis, increased extramedullary hematopoiesis, and/or hepatic congestion as a result of decreased congenital heart function.[38] In this study, findings from post-treatment serial fetal ultrasounds showed the most severe abnormalities, such as hydrops, are typically the first abnormalities to resolve, with slower resolution of placentomegaly and hepatomegaly (Figure 10).[37]
Treatment of Syphilis During Pregnancy
Treatment of syphilis in pregnancy has two main goals: (1) to cure syphilis in the pregnant woman and (2) to prevent (or cure) T. pallidum infection in the fetus.[39] For pregnant women with any stage of syphilis, parenteral penicillin G is the only antimicrobial that has documented efficacy for the treatment of fetal infection.[19,40] Therefore, all pregnant women with a diagnosis of syphilis should receive treatment with penicillin, with the exact regimen based on the syphilis stage.[19] The results of fetal ultrasound do not change syphilis treatment for the mother. In addition, the treatment for syphilis is the same in pregnant women as for adults who are not pregnant, with a few key differences as outlined below (Figure 11). Detailed treatment recommendations based on the stage of syphilis are provided in the sections below.[16,19]
- There are no recommended penicillin alternatives when treating syphilis in pregnant women.
- When treating primary, secondary, and early latent syphilis during pregnancy, some experts recommend giving an extra (second) dose of benzathine penicillin G 2.4 million units 1 week after the initial dose. This recommendation is strongest for women who have reached the 20th gestational week of the pregnancy.
- When treating late latent syphilis (or latent syphilis of unknown duration) in pregnant women, the allowed gap with the 3-dose weekly regimen is more stringent when treating pregnant women: any dose that is not given within 9 days is considered a missed dose, and the 3-dose weekly regimen must be started over.
- The Jarisch-Herxheimer reaction has enhanced importance in pregnancy since it may cause premature labor and potential complications in the fetus, including fetal death. The impact of the Jarisch-Herxheimer reaction is greatest among women who have reached gestation week 20 of the pregnancy and when the woman has early-stage syphilis that is treated during the first or second trimesters.
Treatment of Primary and Secondary Syphilis in Pregnancy
The treatment of primary and secondary syphilis is the same for pregnant women as for adults who are not pregnant, but, for pregnant women, some experts recommend giving a second dose of intramuscular benzathine penicillin G 2.4 million units 1 week after the initial penicillin dose, especially when syphilis is treated after 20 weeks of pregnancy (Table 1).[16,19,41,42,43] The rationale for considering a second penicillin dose in this setting is based on theoretical considerations related to volume expansion and pharmacokinetic changes that occur during pregnancy, which result in reduced penicillin levels, especially in the second half of pregnancy.[44,45] Note that the risk of Jarisch-Herxheimer reaction, which may be highly problematic during pregnancy, is more likely to occur following the treatment of individuals who have early syphilis (primary, secondary, or early latent).
Treatment of Latent Syphilis During Pregnancy
The treatment of pregnant women with latent syphilis requires appropriate classification into early latent syphilis (acquired less than 1 year ago) or late latent syphilis (acquired longer than 1 year ago); treatment of latent syphilis of unknown duration is the same as for late latent syphilis (Table 2).[19]
- Treatment of Early Latent Syphilis: Early latent syphilis is treated with intramuscular benzathine penicillin G 2.4 million units given as a single dose. Similar to the approach for treating primary and secondary syphilis in pregnant women, some experts would give a second dose of intramuscular benzathine penicillin G 2.4 million units 1 week after the initial penicillin dose to treat early latent syphilis, especially when syphilis is treated after 20 weeks gestation.
- Treatment of Late Latent Syphilis (or Latent Syphilis of Unknown Duration): The treatment of late latent syphilis (or latent syphilis of unknown duration) in pregnant women consists of benzathine penicillin G 2.4 million units given every 7 days for a total of 3 doses (7.2 million units total). For pregnant women receiving this series of 3 benzathine penicillin injections, it is important to stay exactly on schedule with the doses spaced 7 days apart. Any benzathine penicillin dose that is not given within 9 days of the prior dose is considered a missed dose, and the entire 3-dose series must be started over.[19,44]Check-on-Learning QuestionWhat should be recommended now for the penicillin treatment?Check
-On-
Learning
QuestionA 27-year-old pregnant woman is diagnosed with late latent syphilis in pregnancy. She received the first of three doses of 2.4 million units of intramuscular benzathine penicillin G. She was supposed to receive the second dose 1 week later, but she returned 10 days after her first dose.What should be recommended now for the penicillin treatment?
Treatment of Neurosyphilis, Ocular Syphilis, or Otosyphilis During Pregnancy
The recommended treatment regimen for neurosyphilis, ocular syphilis, and/or otosyphilis during pregnancy is aqueous crystalline penicillin G (18-24 million units per day, given as 3-4 million units intravenously every 4 hours, or as a continuous infusion, for a total of 10 to 14 days) (Table 3).[19] Note: Procaine penicillin G is no longer available for use. Therefore, treatment of neurosyphilis, ocular syphilis, and/or otosyphilis during pregnancy always consists of intravenous aqueous penicillin G, which usually requires hospitalization and careful monitoring. Some experts recommend giving additional therapy (with one dose of intramuscular benzathine penicillin G 2.4 million units) after completing the 10-14 day intravenous penicillin G regimen, in order to provide a total duration of therapy comparable to the treatment duration used for late latent syphilis; there are, however, no data to support this approach.
Treatment of Tertiary Syphilis During Pregnancy
In the modern era, a diagnosis of tertiary syphilis is rare, particularly among pregnant women. All persons diagnosed with tertiary syphilis, including pregnant women, should undergo a neurologic assessment and a lumbar puncture with cerebrospinal fluid analysis, since this will determine the specific therapy. Some experts recommend treating all persons who have cardiovascular manifestations of tertiary syphilis with a neurosyphilis regimen.
- Treatment of Tertiary Syphilis During Pregnancy (without Evidence of Neurosyphilis): If the findings of the neurologic assessment are negative and the cerebrospinal fluid analysis is normal, then treatment of tertiary syphilis in pregnancy is the same as used for treatment of late latent syphilis: Benzathine penicillin G 2.4 million units given every 7 days for a total of 3 doses (7.2 million units total). For pregnant women, any benzathine penicillin dose that is not given within 9 days of the prior dose is considered an unacceptable gap in treatment, and the entire 3-dose series must be started over.
- Treatment of Tertiary Syphilis During Pregnancy (with Evidence of Neurosyphilis): If the findings of the neurologic assessment and cerebrospinal fluid analysis suggest a diagnosis of neurosyphilis, then treatment is the same as that given for neurosyphilis during pregnancy: Aqueous crystalline penicillin G (18-24 million units per day, given as 3-4 million units intravenously every 4 hours, or as a continuous infusion, for a total of 10 to 14 days).
Management of Pregnant Women Exposed to a Sex Partner with Syphilis
All pregnant women who report contact with a sex partner who has been diagnosed with syphilis should have prompt clinical evaluation for any syphilis-related clinical signs or symptoms, serologic testing for syphilis, and presumptive treatment of early syphilis. If no clinical manifestations of syphilis are observed, then empiric treatment for early syphilis (one dose of intramuscular benzathine penicillin G 2.4 million units) should be administered to the pregnant woman. In this situation, we recommend giving a dose of penicillin to the patient regardless of their partner’s stage of syphilis or how much time has passed since the sexual contact. If the pregnant woman does not have any syphilis-related manifestations and the serologic syphilis testing is positive, and the circumstances indicate a diagnosis of late latent syphilis (or latent syphilis of unknown duration), then the treatment should be adjusted to benzathine penicillin G 2.4 million units given every 7 days for a total of 3 doses (7.2 million units total).
Treatment of Syphilis in Pregnancy in Persons Allergic to Penicillin
For pregnant women with any stage of syphilis, parenteral penicillin G is the only antimicrobial that has documented efficacy for the treatment of fetal infection.[19,40] Therefore, any pregnant woman with a reported penicillin allergy who is diagnosed with syphilis should promptly undergo a thorough evaluation of reported allergy symptoms, as most individuals with reported penicillin allergy do not have a serious allergic reaction that would prevent treatment of syphilis with penicillin. Suspicion or verification of an IgE-mediated or other life-threatening reaction to penicillin should prompt immediate referral to an allergist to (1) better characterize the penicillin allergy, (2) perform penicillin skin testing if indicated, and (3) conduct penicillin desensitization if indicated.[19] Penicillin desensitization should be followed immediately by treatment with penicillin based on the syphilis stage; desensitization does not need to be repeated if the treatment course is completed without missed doses. If any dose in a prescribed treatment course of intramuscular benzathine penicillin G is missed, the desensitization protocol must be repeated. In pregnant women with documented penicillin allergy, oral and intravenous penicillin desensitization protocols have been successfully used.[46,47] Evaluation, referral, and potential allergy testing and desensitization should be considered urgent to avoid delays in treatment of syphilis in pregnancy, which could increase the risk for pregnancy complications and congenital infection.
Jarisch-Herxheimer Reaction in Pregnancy
General Description of Jarisch-Herxheimer Reaction
The Jarisch-Herxheimer reaction is a self-limited reaction associated with the initiation of antitreponemal therapy. This reaction represents a systemic inflammatory response following the antimicrobial treatment of T. pallidum—it is not an allergic reaction to penicillin. Pregnant women undergoing treatment for syphilis have an estimated 20-45% risk of developing a Jarisch-Herxheimer reaction, with the highest rates after treatment of early syphilis and when treatment is initiated after 20 weeks' gestation.[19] When this reaction occurs, it typically begins within several hours after the first treatment dose of penicillin and nearly always within 24 hours. The Jarisch-Herxheimer reaction is characterized by fever, malaise, nausea, vomiting, and, less frequently, chills, hypotension, or an exacerbation of a secondary syphilis rash.[48,49] This reaction can be mistaken for an allergic reaction to penicillin.
Management of Jarisch-Herxheimer Reaction in Pregnancy
If the Jarisch-Herxheimer reaction occurs during the second half of pregnancy, it has the potential to cause fetal complications, including fetal heart rate abnormalities, premature labor, and, rarely, fetal death.[16,49,50] The reported frequency of this reaction after syphilis treatment in pregnancy has ranged from 5-40% and occurs most frequently when findings on ultrasound indicate severe congenital infection.[49,50] All pregnant women initiating syphilis treatment should receive counseling about the potential occurrence of a Jarisch-Herxheimer reaction. When initiating syphilis treatment in a pregnant woman, after fetal viability with findings on ultrasound suggesting congenital infection, some experts recommend administering the first dose of penicillin in a labor and delivery unit with continuous fetal heart rate monitoring for 24 hours.[16] Pregnant women initiating syphilis treatment in the second half of pregnancy who are not monitored in a clinic or hospital setting should receive counseling to promptly seek obstetric medical care if they develop any fever, contractions, or decrease in fetal movements; monitoring for these symptoms is especially important in the first 24 hours after receiving syphilis treatment.[19] There is no specific management for the Jarisch-Herxheimer reaction other than providing supportive care, which includes antipyretics and intravenous fluids; corticosteroids are not recommended. Typically, the reaction resolves within 24 hours.[20]
Efficacy of Syphilis Treatment During Pregnancy
The efficacy of syphilis treatment during pregnancy is judged both for the success rate of eradicating maternal infection and in preventing congenital syphilis. Available data suggest that appropriate treatment of syphilis during pregnancy is highly effective, with a success rate of greater than 99% in eradicating maternal T. pallidum infection and a greater than 98% success rate in preventing congenital syphilis.[8,14,16,40,42,44,51]
Efficacy Based on Syphilis Stage
The best data for treatment efficacy comes from a prospective evaluation of 340 women diagnosed with syphilis during pregnancy at Parkland Hospital in Dallas, Texas, in 1987-1989.[40] Treatment of syphilis resulted in an overall maternal success rate of 99.7% (339 of 340), with success defined as eradicating maternal disease.[40] In addition, maternal syphilis treatment had a 98.2% (334 of 340) success rate in preventing congenital syphilis.[40] The success rate in preventing congenital syphilis was very high regardless of the maternal syphilis stage of syphilis, but the rate of congenital syphilis was slightly lower when treatment was administered to women with secondary syphilis.[40] Of note, when examining the success rate for all early syphilis stages (primary, secondary, and early latent), which are the stages most likely to result in transmission of T. pallidum to the fetus, the success rate remained very high at 97.1% (198 of 204).[40]
Table 4. Success of Maternal Treatment of Syphilis in Preventing Congenital Syphilis, by Maternal Syphilis Stage
Maternal Syphilis Stage Success* / Total Treated Percentage Success* Primary 27/27 100% Secondary 71/75 94.7% Early Latent 100/102 98.0% Late Latent 136/136 100% All Stages 334/340 98.2% *Success defined as preventing congenital syphilis
Source:- Alexander JM, Sheffield JS, Sanchez PJ, Mayfield J, Wendel GD Jr. Efficacy of treatment for syphilis in pregnancy. Obstet Gynecol. 1999;93:5-8. [PubMed Abstract]
Efficacy Based on Gestational Age
In the same prospective evaluation discussed above, investigators demonstrated that the success rate in preventing congenital syphilis was high throughout the pregnancy, but slightly lower if the diagnosis occurred very late in the pregnancy, particularly after a gestational age of 36 weeks.[40] The higher rates of congenital syphilis associated with late gestational age is thought to result from a combination of factors, including the shorter interval between treatment and delivery (which would allow for less time to see treatment results), late gestation diagnosis possibly reflecting longer fetal infection, and potential physiologic changes that take place later in pregnancy that could reduce penicillin levels.[39]
Table 5. Success of Maternal Treatment of Syphilis in Preventing Congenital Syphilis, by Gestational Age
Gestational Age Success* / Total Treated Percentage Success* ≤20 weeks 152/153 99.4% 21-25 weeks 51/51 100% 26-30 weeks 58/59 98.3% 31-35 weeks 44/46 95.6% 36-40 weeks 26/28 92.9% 41-42 weeks 3/3 100% All Gestational Ages 334/340 98.2% *Success defined as preventing congenital syphilis
Source:- Alexander JM, Sheffield JS, Sanchez PJ, Mayfield J, Wendel GD Jr. Efficacy of treatment for syphilis in pregnancy. Obstet Gynecol. 1999;93:5-8. [PubMed Abstract]
Follow-Up of Women Treated for Syphilis During Pregnancy
Follow-Up After Treating Syphilis During Pregnancy
The clinical and laboratory and clinical follow-up after treating syphilis in pregnant women is extremely important. In addition to monitoring and follow-up for the fetus and infant, post-treatment follow-up for pregnant women has two primary objectives: (1) to document an appropriate serologic response to therapy and (2) to monitor for evidence of reinfection with T. pallidum. Note that an adequate clinical and/or serologic response in the pregnant mother does not confirm the absence of neonatal infection.[3] In addition, if syphilis treatment occurs within 30 days of delivery, the risk of congenital syphilis is increased compared with treatment earlier in the pregnancy, even if the mother has an excellent clinical and serologic response to syphilis treatment.[19,52]
Clinical Follow-Up
- Immediate Post-Treatment Monitoring: Development of a Jarisch-Herxheimer reaction can precipitate uterine contractions, preterm labor, and/or fetal distress, particularly for women beyond 20 weeks’ gestation who have early syphilis infection with evidence of congenital infection.[16,45] Therefore, pregnant women treated for syphilis in the second half of pregnancy should receive counseling to closely self-observe for 24–48 hours after treatment for an acute febrile reaction, uterine contractions, and decreased fetal movement. The intensity and type of immediate post-treatment monitoring vary. Identifying the best location for treatment and the necessity of fetal monitoring should be determined in consultation with experts, and the inability to provide fetal monitoring should not delay the administration of initial penicillin treatment.[3,45,53] Some centers administer the first dose of penicillin in a labor and delivery unit, with continuous fetal monitoring for at least 24 hours after the dose of penicillin has been administered.[16,36,45] Most experts would agree that intensive monitoring is recommended if the mother develops any signs or symptoms to suggest a Jarisch-Herxheimer reaction.
- Subsequent Clinical Follow-Up: Post-treatment clinical follow-up should include a physical examination to evaluate the resolution of clinical syphilis-related manifestations. For pregnant women with genital syphilitic lesions (chancre, mucous patches, or condylomata lata), reevaluation of the lesions is especially important, since infant contact with unresolved genital syphilitic lesions could occur during birth and result in transmission of T. pallidum from the mother to the newborn.[3] For pregnant women diagnosed with latent syphilis, there are no clinical findings to reevaluate.
Syphilis Serologic Testing Follow-Up
All pregnant women diagnosed with syphilis should have a baseline quantitative nontreponemal titer (RPR or VDRL), which serves as a benchmark for comparison with subsequent post-treatment nontreponemal titers.[19] In addition, the same type of nontreponemal test (RPR or VDRL) should consistently be used to compare the quantitative titers, since these tests are not equivalent and RPR titers are typically slightly higher than VDRL titers.[26] For adult non-pregnant patients, follow-up syphilis serologic testing typically occurs 6 months after treatment, but for pregnant women, follow-up testing is performed much earlier, ideally after 8 weeks. The main reason for not waiting 6 months for repeat testing is the urgency of documenting effective treatment to prevent congenital syphilis. Testing sooner than 8 weeks should be performed if there are clinical manifestations to suggest reinfection and a new diagnosis of syphilis.[19] The post-treatment syphilis serologic monitoring schedule during pregnancy depends on whether the syphilis treatment was initiated before or after week 24 of gestation. A maternal follow-up nontreponemal titer at birth is always recommended, regardless of when the most recent titer was obtained, since this titer is used to compare with newborn titers.
- Initial Repeat Testing for Pregnant Women Treated At or Before Week 24 Gestation: If syphilis treatment is initiated at or prior to week 24 gestation, subsequent nontreponemal serologic testing should occur 8 weeks after treatment initiation and then again at birth. For example, a pregnant woman who has syphilis treatment initiated at 22 weeks’ gestation should have syphilis serologic testing repeated at week 30 gestation and again at birth. Obtaining a birth nontreponemal titer is always recommended, regardless of when the most recent titer was obtained, since this birth maternal titer is used to compare with newborn titers.
- Initial Repeat Testing for Pregnant Women Treated After Week 24 Gestation: If syphilis treatment occurred after 24 weeks’ gestation, subsequent nontreponemal serologic testing should occur at birth. For example, a pregnant woman who has syphilis treatment initiated at 27 weeks’ gestation should have syphilis serologic testing repeated at birth. Typically, repeat syphilis nontreponemal titers should not be performed within 8 weeks of the prior titer, but if syphilis treatment was initiated very late in pregnancy, the birth nontreponemal serologic test should still occur, even if less than 8 weeks have elapsed from treatment initiation. The birth nontreponemal titer should always be obtained, regardless of the timing of the most recent titer, since the maternal titer at birth is used to compare with newborn titers.
- Automated or State-Required Third Trimester Syphilis Screening: Repeat syphilis serologic testing that is automated by electronic record protocols or required by state law in the third trimester can complicate follow-up nontreponemal test scheduling. In this situation, an additional syphilis “screening” serologic test may be unnecessarily performed, but extra testing is preferable to missed follow-up testing.
- Follow-Up Monitoring After Birth: Mothers treated for syphilis during pregnancy should continue to have nontreponemal serologic monitoring after delivery to evaluate and document their response to therapy. More than 50% of pregnant women treated for syphilis will not achieve a 4-fold decline in nontreponemal titer during pregnancy, especially women treated for syphilis late in the pregnancy, which underscores the need for monitoring after delivery.[45,54] The lack of a 4-fold decline by delivery has been associated with older maternal age, latent syphilis, and less time from treatment to delivery.[54]Check-on-Learning QuestionWhat is recommended for syphilis post-treatment serologic follow-up testing during pregnancy?Check
-On-
Learning
QuestionA 19-year-old woman is diagnosed with secondary syphilis at gestation week 19 and has reactive treponemal tests and nontreponemal test (RPR titer 1:64). She immediately received 1 dose of 2.4 million units of benzathine penicillin G given as an intramuscular dose.What is recommended for syphilis post-treatment serologic follow-up testing during pregnancy?
Interpreting Nontreponemal Titer Changes and Response to Therapy
Changes in nontreponemal titers (RPR or VDRL) are described quantitatively as a “fold” decrease or increase, based on the comparison between the most recent nontreponemal titer and previous titers using the same type of nontreponemal test. In general, a 4-fold or greater change in titer (e.g., from 1:32 to 1:8 or from 1:8 to 1:32) is considered clinically significant (if the same type of nontreponemal test was used). The following summarizes standard definitions for categories of treatment responses.
- Adequate Serologic Response / Serologic Cure: A post-treatment 4-fold or greater decrease in titer is considered an adequate serologic response if it occurs in the expected timeframe after treatment (6-12 months for primary or secondary syphilis, 12–24 months for latent syphilis, and 24 months for any stage of syphilis in persons with HIV).[55] This is also referred to as serologic cure.[55]
- Seroreversion: The term seroreversion refers to persons who have a nonreactive post-treatment nontreponemal titer (RPR or VDRL).
- Serologic Response with Lack of Seroreversion: Frequently, people treated for syphilis will have a 4-fold decline in nontreponemal titers (RPR or VDRL) but have a persistently elevated titer. For example, a pregnant woman has a good response to adequate syphilis treatment with an 8-fold decline in titer (pretreatment RPR titer of 1:128 decreases to 1:16). Further follow-up RPR titers remain elevated at 1:18 and 1:16. This situation would be considered a serologic response with lack of seroreversion. In this scenario, available data suggest no benefit from giving additional antimicrobial therapy, unless re-exposure or reinfection is suspected.[55]
- Serologic Nonresponse / Inadequate Serologic Response: A serologic nonresponse (or inadequate serologic response) is defined as the absence of a fourfold or greater decline in nontreponemal titers following treatment within the expected timeframe: 12 months for primary or secondary syphilis, 24 months for latent syphilis, and 24 months for any stage of syphilis in individuals with HIV.[55]
- Serofast: The term serofast was historically defined as a person who had resolution of syphilis-related clinical manifestations after syphilis treatment, but who failed to achieve a nonreactive nontreponemal test. In the modern era, the term serofast has been modified to include persons with (1) a post-treatment 4-fold or greater decline in titer, but with persistent reactive nontreponemal tests in the expected timeframe, and (2) failure to achieve a 4-fold or greater decline in the expected timeframe.[26,55] Some experts and clinicians have also used the term serofast to describe persons who have an adequate serologic response after syphilis treatment (greater than 4-fold decline in nontreponemal titers), but have a persistently poistive low-level nontreponemal titer (typically the RPR or VDRL remains elevated at a titer <1:8).[26,#]
Clinical Manifestations of Syphilis in Neonates and Young Children
Congenital Syphilis
Untreated syphilis during pregnancy may result in a wide range of outcomes, including infant death, stillbirth, birth of an infant with clinical signs or symptoms of congenital syphilis, and birth of an infant with no documented signs or symptoms of congenital syphilis.[56] Transmission to the fetus in pregnancy can occur during any stage of syphilis, but the risk is much higher with early syphilis.[3,7,16] Fetal infection can occur during any trimester of pregnancy. Congenital syphilis is traditionally classified as either early or late disease.[59] Early manifestations occur within the first two years of life, and late manifestations occur after two years of age. Although infants with congenital syphilis most often display some early manifestations, some do not have clinical manifestations of active disease at the time of birth or early in life. The following summarizes the common clinical manifestations observed with early congenital syphilis and late congenital syphilis.[12,60,61,62]
Early Congenital Syphilis
Early congenital syphilis is usually defined as manifestations of syphilis in infants and children younger than 2 years of age, with more common abnormalities that include the following:[3,12,60,63]
- Small for gestational age
- Rhinitis (snuffles)
- Jaundice
- Hepatomegaly
- Splenomegaly
- Lymphadenopathy
- Skin rash (begins as a maculopapular rash and may progress to form bullous or desquamating lesions)
- Bone involvement (osteochondritis, diaphyseal osteomyelitis, periostitis, and pseudoparalysis)
- Ophthalmic disorders (cataracts, chorioretinitis, uveitis, interstitial keratitis, optic neuritis)
- Neurologic (cranial nerve palsies, meningitis, seizures)
- Myocardial dysfunction (myocarditis, congestive heart failure)
- Laboratory abnormalities (anemia, thrombocytopenia, elevated aminotransferase and bilirubin levels)
Activity: Early Congenital SyphilisNavigate this visual guide by using the menu on the left side or by scrolling.(Figure 1)Late Congenital Syphilis
Late congenital syphilis is generally defined as manifestations of syphilis in children older than 2 years of age, which typically result from scarring and chronic inflammatory changes from persistent infection and inflammation, and may manifest with one or more of the following disorders (Figure 12):[12,60,64]
- Facial changes (frontal bossing due to periostitis, saddle deformity of the nose due to destruction of cartilage)
- Perforation of the hard palate
- Abnormal tooth development (Hutchinson’s teeth and mulberry molars)
- Bone abnormalities (shortened maxilla, tibial thickening [saber shins])
- Ophthalmic disorders (interstitial keratitis, glaucoma, optic atrophy)
- Deafness
Screening and Evaluation of Syphilis in Neonates
Routine Screening of Neonates for Syphilis
For neonates born to mothers who have not been diagnosed with syphilis, routine serologic screening for syphilis is not recommended.[19] It is extremely important, however, that no newborn infant is discharged from the hospital until the mother’s syphilis serologic status has been documented at least once.[19] All neonates born to mothers diagnosed with syphilis during pregnancy require evaluation, even if the mother has been adequately treated.
Evaluation of Infants Born to Mothers Diagnosed with Syphilis
All infants born to mothers who were diagnosed with syphilis should undergo clinical evaluation and serologic testing. In some instances, the evaluation of these neonates may include hematologic evaluation, evaluation for hepatobiliary dysfunction, radiographic evaluation for long-bone deformities, and cerebrospinal fluid evaluation for neurosyphilis. The specific evaluation depends on the four categories of risk for congenital syphilis: (1) confirmed proven or highly probable congenital syphilis; (2) possible congenital syphilis; (3) congenital syphilis less likely; and (4) congenital syphilis unlikely.[19] No evaluation is recommended for the latter two categories (when congenital syphilis is less likely or unlikely).[19] The criteria for each of these categories and the recommended approach and treatment are discussed in detail in the next section on Management of Syphilis in Neonates and Young Children.
Clinical Evaluation
All neonates born to a mother diagnosed with syphilis should have a thorough physical examination.[19] Diagnosing congenital syphilis, based on physical examination findings, can be challenging, since syphilis can cause a broad array of clinical manifestations, as outlined in the previous section on Clinical Manifestations of Syphilis in Neonates and Young Children. Findings from the physical examination are essential to inform syphilis treatment decisions for the neonate. Common syphilis-related signs that should be assessed include persistent nasal discharge (snuffles), bullous or maculopapular skin rash (often involving palms and soles), desquamation of the hands and feet, hepatomegaly, splenomegaly, and cranial nerve palsies.[12,62]
Serologic Syphilis Testing
The serologic diagnosis of syphilis in infants is often difficult, since maternal nontreponemal and treponemal IgG antibodies are passively transferred through the placenta to the fetus and may confound results, especially in the first 30 days of life.[3,19] Therefore, neonates undergoing evaluation for syphilis should undergo testing with a quantitative nontreponemal test (RPR or VDRL), and the test should be performed on a serum sample; the use of umbilical cord blood for syphilis testing is not recommended since it may be contaminated with maternal blood, which could lead to a false-positive result.[19] It is important to use the same type of nontreponemal test (RPR or VDRL) for serologic testing of the neonate and the mother’s test obtained at birth.[19,26] A neonate nontreponemal titer that is 4-fold or greater than the maternal titer (using the same type of nontreponemal test) meets the serologic diagnostic criteria for congenital syphilis.[3,19]
Direct Detection Tests for Treponema pallidum
Methods to directly detect T. pallidum, such as nucleic acid amplification tests (NAATs), immunohistochemistry, silver staining, or darkfield microscopy, are available in some medical centers, but these methods are not routinely recommended for the standard evaluation of neonates born to mothers who have been diagnosed with syphilis. If these direct detection methods are available, they can be used to make a diagnosis of syphilis: a positive darkfield test or polymerase chain reaction (PCR) of placenta, cord, lesions, or body fluids (or a positive silver stain of the placenta or cord) meets the criteria for confirmed proven or highly probable congenital syphilis.
- NAAT: At this time, there are no FDA-cleared NAATs for the diagnosis of syphilis. Several laboratories have developed Clinical Laboratory Improvement Amendments (CLIA)-validated NAATs and multiple NAATs have been used in research studies. Available data show that NAATs, when compared with a gold standard rabbit infectivity test, have a sensitivity of 60% versus 75% for neonatal CSF and 67% versus 94% with neonatal whole blood or serum.[51,65,66] The 2021 STI Treatment Guidelines suggest that a CLIA-validated NAAT could be considered for examination of the placenta, umbilical cord, or the neonate (nasal discharge, a suspicious lesion, or other body fluids.[19]
- Immunohistochemistry: The use of immunohistochemistry is preferred over silver-staining for formalin-fixed tissue specimens, such as placental tissue or umbilical cord tissue.[26] Immunohistochemistry to detect T. pallidum in placental tissue infection has an estimated sensitivity of 68-82% and specificity of 58%.[67] If immunohistochemistry is used to test placental tissue, the specimen should be taken at the periphery of the placenta, close to where the cord is attached.[26] If immunohistochemistry is performed on the umbilical cord, a sample approximately 3–4 cm long should be obtained immediately after delivery (from a section distal to the placenta).[26] The umbilical cord should not be cleaned with any antimicrobial solution prior to collecting the sample.[26] With sampling of the placenta or umbilical cord, the tissue should be fixed in 10% buffered formalin at room temperature.[26] Clinical pathologists can provide rapid results confirming a diagnosis of congenital syphilis—using immunohistochemical testing of umbilical cord sections—when the infant is suspected to have congenital syphilis, or when untreated maternal syphilis is diagnosed at the time of delivery.
- Darkfield Microscopy: In clinical settings, darkfield microscopy is rarely used for diagnosing congenital syphilis for multiple reasons: most hospitals do not have a darkfield microscope, few people have proficiency with darkfield microscopy, the test should optimally be done using serous fluid free of red blood cells, and the test must be performed within 20 minutes of the sample collection otherwise spirochete motility is compromised.[26] If darkfield microscopy is available for diagnosing congenital syphilis, it has the most potential benefit when evaluating neonates with nasopharyngeal discharge (“snuffles”) or moist cutaneous lesions, such as a bullous rash.[26]
Laboratory Evaluation
- HIV Testing: All neonates who have a mother diagnosed with syphilis should undergo HIV testing (as soon as possible after the maternal diagnosis of syphilis is known).[19] In addition, routine screening for HIV is recommended for all pregnant women.
- Complete Blood Count (CBC) and Differential: Neonates may have multiple hematologic abnormalities, including anemia, elevated white blood cell counts, and thrombocytopenia.[12] Ordering a CBC is recommended for all neonates with either (1) confirmed proven or highly probable congenital syphilis and (2) possible congenital syphilis.
- Liver Function Tests: Among infants with symptomatic congenital syphilis, hepatobiliary abnormalities are common. Liver function tests, including alanine aminotransferase (ALT), aspartate aminotransferase (AST), alkaline phosphatase, and total bilirubin, should be considered if clinically indicated for neonates with confirmed proven or highly probable congenital syphilis.
Radiographic Evaluation
- Long Bone Radiographs: Congenital syphilis may manifest with bone deformities that are apparent on radiographic examination. Typical abnormalities include lesions in the long bones that have a moth-eaten appearance that is a result of bone demineralization, fractures, or periosteal reactions.[12,68,69] Radiographic evaluation of long bones in neonates typically consists of bilateral imaging of the femur, tibia, and fibula.[62] The presence of moth-eaten deformities is considered diagnostic for congenital syphilis. Some bone manifestations, such as those that occur with osteochondritis or periostitis, may not manifest radiographically until 5 or 16 weeks, respectively, after fetal infection.
- Neuroimaging: Routine neuroimaging is not recommended but may be indicated in neonates with seizures, suspected meningitis, and/or a focal neurologic examination.
Management of Neonates and Young Children Born to Mothers Diagnosed with Syphilis
Among infants born to mothers diagnosed with syphilis, the evaluation and treatment decisions for the management of congenital syphilis are complex and should ideally include a clinician and/or specialist who has significant expertise in managing congenital syphilis. If this is not possible, expert consultation should be obtained. Note that if maternal syphilis treatment occurs within 30 days of delivery, treatment failure is more likely, and if infection occurs, the infant may have asymptomatic T. pallidum infection. The evaluation and management of neonates born to mothers diagnosed with syphilis depends on the likelihood that the neonate/young child has congenital syphilis. To determine the likelihood of congenital syphilis, the following factors should be taken into account:
- Maternal history of T. pallidum infection (when diagnosed in pregnancy, stage of syphilis at diagnosis, and fetal ultrasound findings)
- Treatment of syphilis in the mother (regimen and when in pregnancy)
- Evaluation of the neonate (physical examination findings, laboratory abnormalities, radiographic abnormalities in long bones)
- The neonate/child’s nontreponemal test results and titer compared with the mother’s nontreponemal titer (both obtained at birth)
Antimicrobial Therapy for Treating Congenital Syphilis
For the treatment of neonatal syphilis, there are inadequate data on the use of antimicrobial therapy other than penicillin. Procaine penicillin G is no longer available in the United States and thus is not an option. The treatment of congenital syphilis is the same in neonates with or without HIV infection. In addition, the antimicrobial treatment of congenital syphilis is not altered by the mother’s HIV status.
Adjustment of Penicillin Dosing Based on Age in Neonates
The recommendation to adjust the penicillin dosing frequency (and increase the daily dose) after 7 days of life is based on major changes in neonatal renal clearance of penicillin that occur very early in life. Penicillin is almost entirely cleared renally via tubular secretion and in very young neonates (younger than 7 days) there is poor penicillin renal tubular secretion due to reduced peritubular blood flow, short tubule length, diminished concentrating ability, and decreased transporter expression. This reduced penicillin clearance can potentially result in the accumulation of penicillin and thus the need for less frequent dosing. For infants who are older than 7 days, renal clearance increases and there is less penicillin accumulation. Therefore, for infants older than 7 days of age, the penicillin dose is adjusted and increased by altering the dosing from every 12 hours to every 8 hours. The total duration of treatment is 10 days.
Penicillin Allergy
Since penicillin is the only antimicrobial with established efficacy for treating congenital syphilis, neonates, infants, and children who require treatment for congenital syphilis but who have a history of penicillin allergy or develop an allergic reaction presumed secondary to penicillin should undergo penicillin desensitization and receive treatment with penicillin G.[19] Expert consultation with or management by an allergy specialist and an infectious diseases expert is recommended. Ceftriaxone (in doses for age and weight) has been used in situations of penicillin shortages.[19] If ceftriaxone is used, the following doses are recommended: (1) for infants 30 days of age and older, use ceftriaxone 75 mg/kg body weight/day IV or IM in a single daily dose for 10–14 days (dose adjustment might be necessary on the basis of current weight); (2) for children, the recommended ceftriaxone dose is 100 mg/kg body weight/day in a single daily dose.[19] If a regimen other than penicillin is used to treat congenital syphilis, close clinical and serologic follow-up should occur.[19]
Evaluation of Neonates Born to Mothers Diagnosed with Syphilis During Pregnancy
Based on the review of all the factors outlined above, neonates born to mothers diagnosed with syphilis are classified into one of four categories: (1) proven or highly probable congenital syphilis, (2) possible congenital syphilis, (3) congenital syphilis is less likely, or (4) congenital syphilis is unlikely.[19] The following will outline each of these four scenarios, followed by a brief discussion of additional scenarios related to maternal syphilis serologic testing (Figure 13).[19]
Category 1: Confirmed Proven or Highly Probable Congenital Syphilis
A neonate is considered to have confirmed proven or highly probable congenital syphilis with any of the following:
- Abnormal physical examination consistent with congenital syphilis, or
- Serum quantitative nontreponemal serologic titer that is fourfold (or greater) higher than the mother’s titer at delivery, or
- A positive darkfield test or PCR of placenta, cord, lesions, or body fluids or a positive silver stain of the placenta or cord.
Recommended Evaluation
The recommended evaluation for neonates with confirmed proven or highly probable congenital syphilis is:
- CSF analysis for VDRL, cell count, and protein
- Complete blood count (CBC) with differential, and platelet count
- Long-bone radiographs
- Other tests as clinically indicated (e.g., chest radiograph, liver function tests, neuroimaging, ophthalmologic examination, and auditory brain stem response)
Recommended Treatment
The recommended treatment for neonates with confirmed proven or highly probable congenital syphilis is a 10-day course of intravenous aqueous crystalline penicillin G. The lower total daily penicillin dosing during the first 7 days of life is based on the significantly reduced neonatal renal clearance of penicillin during the first 7 days of life. A full 10-day course of penicillin is preferred, even if another beta-lactam, such as ampicillin or cefotaxime, was initially administered for another reason, such as possible sepsis or neonatal meningitis.
Table 6. 2021 STI Treatment Guidelines: Congenital SyphilisTreatment of Confirmed or Highly Probable Congenital SyphilisProcaine penicillin G is no longer available in the United States and therefore is not included in this table.Recommended for Treatment of Confirmed or Highly Probable Congenital SyphilisAqueous crystalline penicillin G100,000–150,000 units/kg body weight/day, administered as 50,000 units/kg body weight/dose IV every 12 hours for doses given during the first 7 days of life and every 8 hours thereafter for a total of 10 daysAqueous crystalline penicillin G
Tradename:PfizerpenNote: If more than 1 day of penicillin therapy is missed, the entire course should be restarted.Source: Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021. Syphilis. MMWR Recomm Rep. 2021;70(No. RR-4):1-187. [2021 STI Treatment Guidelines]Category 2: Possible Congenital Syphilis
Congenital syphilis is considered possible with the following:
- The neonate has a normal physical examination, and
- The neonate has a serum quantitative nontreponemal serologic titer that is less than fourfold higher than the maternal titer at delivery, and
- The mother has any one of the following:
- Not treated, inadequately treated, or has no documentation of having received treatment
- Treated with a regimen other than recommended in guidelines
- Received the recommended regimen, but treatment was initiated less than 30 days before delivery
Recommended Evaluation
The recommended evaluation for neonates with possible congenital syphilis includes all the following tests:
- CSF analysis for VDRL, cell count, and protein
- CBC with differential (includes platelet count)
- Long-bone radiographs
The above evaluation is not considered necessary if the infant receives a 10-day treatment course with intravenous aqueous penicillin G, Some experts, however, would recommend doing this evaluation, since certain findings, such as CSF abnormalities, would prompt close follow-up and results from some tests (e.g., CBC, platelet count, and long-bone radiographs) may further support a diagnosis of congenital syphilis. In addition, if the neonate has a nontreponemal test and the mother’s risk for untreated syphilis is low, treatment of the neonate with a single intramuscular dose of benzathine penicillin G 50,000 units/kg body weight for possible incubating syphilis can be considered without an evaluation.
Recommended Treatment
The recommended treatment options for neonates with possible congenital syphilis include a 10-day intravenous aqueous penicillin G option or a single dose of intramuscular benzathine penicillin G. The single-dose benzathine penicillin G intramuscular dose should only be considered if the recommended evaluation has been completed, all results of the evaluation are normal, and follow-up is certain. The 10-day course of intravenous penicillin G is required if any part of the neonate’s evaluation is abnormal or cannot be interpreted (e.g., contamination of CSF with blood), or is not performed. Neonates born to mothers who have untreated early syphilis at the time of delivery are at increased risk of congenital syphilis and should receive a 10-day course of intravenous penicillin, even if the neonate’s nontreponemal test is nonreactive, the complete evaluation is normal, and follow-up is certain.
Table 7. 2021 STI Treatment Guidelines: Congenital SyphilisTreatment of Possible Congenital SyphilisProcaine penicillin G is no longer available in the United States and therefore is not included in this table.Recommended for Treatment of Possible Congenital SyphilisAqueous crystalline penicillin G100,000–150,000 units/kg body weight/day, administered as 50,000 units/kg body weight/dose IV every 12 hours during the first 7 days of life and every 8 hours thereafter for a total of 10 daysAqueous crystalline penicillin G
Tradename:PfizerpenNote: If more than 1 day of penicillin therapy is missed, the entire course should be restarted.Recommended for Treatment of Possible Congenital SyphilisBenzathine penicillin G50,000 units/kg body weight/dose IM in a single doseBenzathine penicillin G
Tradename:Bicillin-LANote: The single-dose benzathine penicillin G intramuscular dose should only be considered if the recommended evaluation has been completed, all results of the evaluation are normal, and follow-up is certain.Source: Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021. Syphilis. MMWR Recomm Rep. 2021;70(No. RR-4):1-187. [2021 STI Treatment Guidelines]Category 3: Congenital Syphilis Less Likely
The diagnosis of congenital syphilis is considered less likely when all the following criteria are met:
- The neonate has a normal physical examination, and
- The neonate has a serum quantitative nontreponemal serologic titer equal to or less than fourfold of the maternal titer at delivery, and
- The mother was treated during pregnancy, treatment was appropriate for the infection stage, and the treatment regimen was initiated ≥30 days before delivery, and
- The mother has no evidence of reinfection or relapse
Recommended Evaluation
When the diagnosis of congenital syphilis is considered less likely for neonates, no evaluation is recommended.
Recommended Treatment
The recommended treatment consists of a single dose of benzathine penicillin G. Another approach involves not treating the newborn if follow-up is certain but providing close serologic follow-up every 2–3 months for 6 months for infants whose mothers’ nontreponemal titers decreased at least fourfold after therapy for early syphilis or remained stable for low-titer, latent syphilis (e.g., VDRL less than 1:2 or RPR less than 1:4).
Table 8. 2021 STI Treatment Guidelines: Congenital SyphilisTreatment When Congenital Syphilis Less LikelyRecommended for Treatment When Congenital Syphilis Less LikelyBenzathine penicillin G50,000 units/kg body weight/dose IM in a single doseBenzathine penicillin G
Tradename:Bicillin-LAAnother approach involves not treating the newborn if follow-up is certain but providing close serologic follow-up every 2–3 months for 6 months for infants whose mothers' nontreponemal titers decreased at least fourfold after therapy for early syphilis or remained stable for low- titer, latent syphilis (e.g., VDRL <1:2 orSource: Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021. Syphilis. MMWR Recomm Rep. 2021;70(No. RR-4):1-187. [2021 STI Treatment Guidelines]Category 4: Congenital Syphilis Unlikely
The diagnosis of congenital syphilis is considered unlikely when all the following criteria are met:
- The neonate has a normal physical examination, and
- The neonate has a serum quantitative nontreponemal serologic titer equal to or less than fourfold of the maternal titer at delivery, and
- The mother was treated during pregnancy, and
- The mother’s nontreponemal serologic titer remained low and stable (i.e., serofast) before and during pregnancy and at delivery (e.g., VDRL ≤1:2 or RPR ≤1:4).
Recommended Evaluation
When the diagnosis of congenital syphilis is considered less likely for neonates, no evaluation is recommended.
Recommended Treatment
No treatment is required. Any neonate who has a reactive nontreponemal test should have serologic follow-up to ensure the nontreponemal test returns to nonreactive. In this situation, a single dose of intramuscular benzathine penicillin G 50,000 units/kg body weight might be considered, particularly if follow-up is uncertain and the neonate has a reactive nontreponemal test.
Check-on-Learning QuestionWhat treatment is recommended for the neonate?Check
-On-
Learning
QuestionA 31-year-old pregnant woman was diagnosed with syphilis at the time of delivery based on a new reactive treponemal and nontreponemal test (RPR titer 1:16). Her neonate has rhinitis and a rash that has early desquamation. The neonate has an RPR titer of 1:128. The neonate is now 2 days old.What treatment is recommended for the neonate?
Additional Scenarios Related to Maternal Syphilis Serologic Testing
There are several specific scenarios that may impact the management of infants who are born to mothers who have syphilis screening performed using an initial treponemal antibody test. Most often, this is considered part of the reverse screening algorithm. The reverse screening algorithm uses treponemal antibody testing (CIA or EIA), followed by nontreponemal testing (RPR or VDRL) for reactive treponemal tests. With this algorithm, additional testing with a second (different) treponemal test is performed if needed to resolve discordant results.
Post-Treatment Reactive Treponemal Test with a Nonreactive Nontreponemal Test
A serologic profile consisting of a reactive treponemal test (e.g., EIA or CIA) and a nonreactive nontreponemal test (e.g., RPR or VDRL) may be observed in women who have received effective syphilis treatment either before or during pregnancy. In this setting, though uncommon, the nonreactive nontreponemal result reflects seroreversion, indicating a strong serologic response to treatment. Rarely, nontreponemal seroreversion can occur in the absence of documented therapy. When this serologic pattern is present, and there is documentation of effective prior treatment with no clinical or serologic evidence of reinfection or relapse, the risk of congenital syphilis is considered to be very low.
- Recommendation: Perform repeat nonreactive nontreponemal (RPR or VDRL) testing of the mother at delivery and evaluate the neonate with a physical examination and nontreponemal (RPR or VDRL) testing.[19] If the mother’s nontreponemal remains nonreactive, the infant’s examination is normal, and the infant’s nontreponemal test is nonreactive, then no further laboratory management or treatment is required.[19]
No Prior Treatment and Reactive Treponemal Test with a Nonreactive Nontreponemal Test
When using the reverse screening algorithm for syphilis serologic testing of a pregnant woman who has no prior history of syphilis treatment, it is possible for her to have a reactive treponemal serologic test (e.g., CIA or EIA) followed by a nonreactive nontreponemal test (RPR or VDRL). In this situation, a second treponemal test (e.g., FTA or TP-PA) is performed. If the only reactive test is the initial treponemal test (CIA or EIA), then the woman is considered to have an isolated reactive treponemal test. In populations with low syphilis prevalence, this most often occurs because of a false-positive result.
- Recommendation: If the neonate’s physical examination is normal and the mother’s risk of syphilis is low, no further evaluation or treatment for syphilis is indicated for the neonate.[19] Repeat testing of the neonate in 4 weeks can be considered, especially if the mother reports any possible recent syphilis exposure.[19]
Isolated Reactive Rapid Treponemal Test at Delivery
For women who are evaluated in labor and have no prior syphilis testing during pregnancy, a point-of-care (rapid) syphilis treponemal test is often performed. A reactive point-of-care treponemal test requires confirmatory laboratory-based testing, including testing with a nontreponemal (RPR or VDRL) assay.
- Recommendation: In this situation, management of the neonate should not be deferred while awaiting the laboratory-based confirmatory syphilis testing.[19] The management of the neonates should follow the same protocol as listed above for neonates with confirmed proven or highly probable congenital syphilis (e.g., perform physical examination, obtain CSF for analysis, and treat with 10 days of intravenous aqueous crystalline penicillin G).[19] If laboratory-based syphilis test results become available while the 10-day treatment is ongoing, the results should be reviewed, and the decision to continue or stop treatment should be made after expert consultation.
Treatment of Infants and Children Older than 1 Month of Age
The recommended treatment for congenital syphilis in infants or children who are at least 1 month of age is aqueous crystalline penicillin G 200,000–300,000 units/kg body weight per day, administered as 50,000 units/kg body weight intravenously every 4–6 hours for 10 days.[19]
Table 9. 2021 STI Treatment Guidelines: SyphilisTreatment of Congenital Syphilis Among Infants and ChildrenInfants and children aged ≥1 month who receive a syphilis diagnosis should have birth and maternal medical records reviewed to assess whether they have congenital or acquired syphilis.Recommended RegimenAqueous crystalline penicillin G200,000–300,000 units/kg body weight/day by IV, administered as 50,000 units/kg body weight every 4–6 hours for 10 daysAqueous crystalline penicillin G
Tradename:PfizerpenIf the infant or child has no clinical manifestations of congenital syphilis and the evaluation (including the CSF examination) is normal, treatment with up to 3 weekly doses of benzathine penicillin G 50,000 units/kg body weight IM can be considered. A single dose of benzathine penicillin G 50,000 units/kg body weight IM up to the adult dose of 2.4 million units in a single dose can be considered after the 10-day course of IV aqueous penicillin G to provide more comparable duration for treatment in those wInfants and children aged ≥1 month with primary or secondary syphilis should be managed by a pediatric infectious disease specialist and evaluated for sexual abuse (e.g. through consultation with child-protection services)Source: Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021. Syphilis. MMWR Recomm Rep. 2021;70(No. RR-4):1-187. [2021 STI Treatment Guidelines]Follow-Up of Neonates and Infants
All neonates born to mothers diagnosed with syphilis should have serologic follow-up, even if they are not treated. In addition, infants with clinical manifestations of syphilis and/or a reactive nontreponemal test should have clinical and syphilis serologic monitoring. The monitoring recommendations are slightly different for neonates (age younger than 30 days) when treated for syphilis than for infants and children (age 1 month or older) when treated. Monitoring older children with acquired syphilis (not congenital syphilis) is not addressed in this lesson.
Monitoring for Neonates
Nontreponemal serologic tests should be used for monitoring neonates; ideally, the same type of nontreponemal test (RPR or VDRL) is used for all comparison tests. Serologic monitoring of neonates should occur every 2–3 months until the nontreponemal test is nonreactive.[19]
- Neonates Treated for Congenital Syphilis: The expectation when infants receive appropriate penicillin treatment for syphilis is that the nontreponemal titer should become nonreactive within 12 months of age.[19] If the nontreponemal titer is still reactive at 12 months of age, reevaluation with CSF analysis should be performed. In this situation, expert consultation is advised as repeat treatment with a 10-day course of parenteral penicillin G may be required.[19]
- Neonates with Untreated Syphilis and Reactive Nontreponemal Test: If the neonate was considered Category 3 (Syphilis less likely) or Category 4 (Syphilis unlikely) and no treatment for syphilis was given, the nontreponemal titers would be expected to decline by 3 months and become nonreactive by 6 months of age.[19] If the titer is nonreactive at 6 months of age, the initial reactive nontreponemal test can be considered a false-positive test result attributed to passive transfer of maternal antibodies, and no further syphilis-related evaluation is needed.[19] If the nontreponemal test has remained reactive at 6 months of age, then treatment of syphilis is indicated, with serologic monitoring after treatment.[19]
- Neonates with Untreated Syphilis and Nonreactive Nontreponemal Test: Neonates who have a nonreactive nontreponemal test and a mother with a reactive nontreponemal test at delivery should have a follow-up nontreponemal titer at 3 months of age.[19] The reason for this recommendation is to rule out serologically negative incubating congenital syphilis at birth.[19] The follow-up syphilis testing should use a nontreponemal test, since treponemal tests can have false-positive results for longer than 15 months due to passive transfer of maternal treponemal IgG antibodies.[19]
- Neonates with Abnormal CSF Studies: Neonates who had abnormal CSF results and received appropriate syphilis treatment do not need routine repeat lumbar puncture with CSF studies.[19] The only reasons for repeating CSF studies are persistently reactive nontreponemal titers after 12 months or new clinical findings that indicate the need for a neurologic work-up. If there is an indication for repeated CSF studies, expert consultation is advised.Check-on-Learning QuestionWhat is the expected nontreponemal serologic response (based on a sample obtained at this visit) that would indicate no further syphilis-related evaluation or treatment is needed for this child?Check
-On-
Learning
QuestionA neonate is appropriately treated for congenital syphilis with intravenous aqueous crystalline penicillin G. At birth, the neonate has a reactive nontreponemal test (RPR titer of 1:256). The infant has a repeat nontreponemal test (RPR) performed at age 13 months.What is the expected nontreponemal serologic response (based on a sample obtained at this visit) that would indicate no further syphilis-related evaluation or treatment is needed for this child?
Post-Treatment Monitoring for Infants
Infants treated for syphilis after the neonatal period (after age 30 days of life) should have clinical and serologic follow-up monitoring every 3 months until the nontreponemal test has declined fourfold or become nonreactive.[19] Infants who do not achieve a fourfold decline in nontreponemal titers after 12–18 months (or conversion of nontreponemal test to nonreactive) or have an increase in nontreponemal titers that persists for longer than 2 weeks should have (1) repeat clinical evaluation and CSF analysis and (2) repeat treatment with a 10-day course of parenteral penicillin G.[19] In this situation, the evaluation and management should occur in consultation with an expert. Note the key differences between the goals for response with infants and neonates are: (1) infants can reach goal with a fourfold decline in titer even if the nontreponemal test remains reactive, whereas neonates are required to have a nonreactive nontreponemal test, and (2) infants have a longer time period to reach this goal (12–18 months) versus 12 months with neonates.[19] The monitoring of older children who acquire syphilis after birth is not addressed in this lesson.
Summary Points
- Cases of congenital syphilis have increased dramatically in recent years, with an approximately 8-fold increase from 2014 to 2023.
- Maternal-fetal transmission of T. pallidum is most likely to occur with early syphilis.
- All pregnant women should undergo routine screening for syphilis. Most experts recommend triple screening, which includes screening at the first health encounter after becoming pregnant, at 28 weeks’ gestation, and at birth.
- Syphilis screening tests include treponemal (antibody) tests, nontreponemal (lipoidal antigen) tests, and point-of-care (antibody) tests.
- For pregnant women diagnosed with syphilis, fetal ultrasound evaluation should be conducted after gestation week 18.
- Penicillin is the only known effective and recommended treatment for syphilis in pregnancy. The penicillin treatment regimen in pregnancy should be based on the stage of syphilis and whether the mother has evidence of neurosyphilis, ocular syphilis, or otosyphilis.
- When ultrasound findings suggest evidence of congenital infection with syphilis, pregnant women who receive syphilis antimicrobial treatment have a significant risk of developing the Jarisch-Herxheimer reaction, which may cause premature labor and rarely fetal death.
- Neonates born to mothers diagnosed with syphilis should undergo careful clinical evaluation and have nontreponemal serologic testing performed.
- The management and treatment of neonates is based on the category of likelihood (proven or highly probable, possible, less likely, unlikely) that the neonate has congenital syphilis.
- Penicillin is the only known effective treatment for congenital syphilis. Treatment dose intervals are adjusted from every 8 hours in the first 7 days of life and every 12 hours after age 7 days.
Check-On-Learning Questions Display Options
These quick questions are meant to keep you on track and check your understanding. They appear throughout the core concepts and are listed here for you to review.Check-on-Learning QuestionWhich one of the following tests should ideally be ordered for the syphilis pregnancy screening test?Check
-On-
Learning
QuestionA 29-year-old woman is seen for her first prenatal visit, and she is about 15 weeks pregnant. She was diagnosed with secondary syphilis 1 year ago and received appropriate treatment. She has a pretreatment nontreponemal RPR titer of 1:128. Six months after treatment, the RPR titer had declined to 1:8. She has not had any additional follow-up syphilis serologic studies.Which one of the following tests should ideally be ordered for the syphilis pregnancy screening test?
Check-on-Learning QuestionWhat should be recommended now for the penicillin treatment?Check
-On-
Learning
QuestionA 27-year-old pregnant woman is diagnosed with late latent syphilis in pregnancy. She received the first of three doses of 2.4 million units of intramuscular benzathine penicillin G. She was supposed to receive the second dose 1 week later, but she returned 10 days after her first dose.What should be recommended now for the penicillin treatment?
Check-on-Learning QuestionWhat is recommended for syphilis post-treatment serologic follow-up testing during pregnancy?Check
-On-
Learning
QuestionA 19-year-old woman is diagnosed with secondary syphilis at gestation week 19 and has reactive treponemal tests and nontreponemal test (RPR titer 1:64). She immediately received 1 dose of 2.4 million units of benzathine penicillin G given as an intramuscular dose.What is recommended for syphilis post-treatment serologic follow-up testing during pregnancy?
Check-on-Learning QuestionWhat treatment is recommended for the neonate?Check
-On-
Learning
QuestionA 31-year-old pregnant woman was diagnosed with syphilis at the time of delivery based on a new reactive treponemal and nontreponemal test (RPR titer 1:16). Her neonate has rhinitis and a rash that has early desquamation. The neonate has an RPR titer of 1:128. The neonate is now 2 days old.What treatment is recommended for the neonate?
Check-on-Learning QuestionWhat is the expected nontreponemal serologic response (based on a sample obtained at this visit) that would indicate no further syphilis-related evaluation or treatment is needed for this child?Check
-On-
Learning
QuestionA neonate is appropriately treated for congenital syphilis with intravenous aqueous crystalline penicillin G. At birth, the neonate has a reactive nontreponemal test (RPR titer of 1:256). The infant has a repeat nontreponemal test (RPR) performed at age 13 months.What is the expected nontreponemal serologic response (based on a sample obtained at this visit) that would indicate no further syphilis-related evaluation or treatment is needed for this child?
Citations
- 1.Hollier LM, Cox SM. Syphilis. Semin Perinatol. 1998;22:323-31.[PubMed Abstract] -
- 2.Machefsky A, Hufstetler K, Bachmann L, Barbee L, Miele K, O'Callaghan K. Rising Stillbirth Rates Related to Congenital Syphilis in the United States From 2016 to 2022. Obstet Gynecol. 2024;144:493-500.[PubMed Abstract] -
- 3.Stafford IA, Workowski KA, Bachmann LH. Syphilis Complicating Pregnancy and Congenital Syphilis. N Engl J Med. 2024;390:242-53.[PubMed Abstract] -
- 4.Centers for Disease Control and Prevention. Sexually Transmitted Infections Surveillance, 2023. Atlanta: U.S. Department of Health and Human Services; 2024.
- 5.McDonald R, O'Callaghan K, Torrone E, et al. Vital Signs: Missed Opportunities for Preventing Congenital Syphilis - United States, 2022. MMWR Morb Mortal Wkly Rep. 2023;72:1269-74.[PubMed Abstract] -
- 6.O'Callaghan KP, Johnson Jones ML, McDonald R, et al. The Congenital Syphilis Prevention Cascade: Reimagining a Missed Prevention Opportunities Framework for Effective Intervention. Sex Transm Dis. 2024;51:8-10.[PubMed Abstract] -
- 7.Wicher V, Wicher K. Pathogenesis of maternal-fetal syphilis revisited. Clin Infect Dis. 2001;33:354-63.[PubMed Abstract] -
- 8.Nathan L, Bohman VR, Sanchez PJ, Leos NK, Twickler DM, Wendel GD Jr. In utero infection with Treponema pallidum in early pregnancy. Prenat Diagn. 1997;17:119-23.[PubMed Abstract] -
- 9.Eallonardo SJ, Freitag NE. Crossing the Barrier: A Comparative Study of Listeria monocytogenes and Treponema pallidum in Placental Invasion. Cells. 2023;13(1):88.[PubMed Abstract] -
- 10.Li W, Yuan W, Huang S, Zou L, Zheng K, Xie D. Research progress on the mechanism of Treponema pallidumbreaking through placental barrier. Microb Pathog. 2023;185:106392.[PubMed Abstract] -
- 11.Peeling RW, Mabey D, Kamb ML, Chen XS, Radolf JD, Benzaken AS. Syphilis. Nat Rev Dis Primers. 2017;3:17073.[PubMed Abstract] -
- 12.Medoro AK, Sánchez PJ. Syphilis in Neonates and Infants. Clin Perinatol. 2021;48:293-309.[PubMed Abstract] -
- 13.Schwartz DA, Larsen SA, Beck-Sague C, Fears M, Rice RJ. Pathology of the umbilical cord in congenital syphilis: analysis of 25 specimens using histochemistry and immunofluorescent antibody to Treponema pallidum. Hum Pathol. 1995;26:784-91.[PubMed Abstract] -
- 14.Wendel GD Jr, Sánchez PJ, Peters MT, Harstad TW, Potter LL, Norgard MV. Identification of Treponema pallidum in amniotic fluid and fetal blood from pregnancies complicated by congenital syphilis. Obstet Gynecol. 1991;78:890-5.[PubMed Abstract] -
- 15.Fiumara NJ, Fleming WL, Downing JG, Good FL. The incidence of prenatal syphilis at the Boston City Hospital. N Engl J Med. 1952;247:48-52.[PubMed Abstract] -
- 16.Rac MW, Revell PA, Eppes CS. Syphilis during pregnancy: a preventable threat to maternal-fetal health. Am J Obstet Gynecol. 2017;216:352-363.[PubMed Abstract] -
- 17.Ho EL, Lukehart SA. Syphilis: using modern approaches to understand an old disease. J Clin Invest. 2011;121:4584-92.[PubMed Abstract] -
- 18.Ghanem KG, Ram S, Rice PA. The Modern Epidemic of Syphilis. N Engl J Med. 2020;382:845-54.[PubMed Abstract] -
- 19.Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021. Syphilis. MMWR Recomm Rep. 2021;70(No. RR-4):1-187.
- 20.Hook EW Rd. Syphilis. Lancet. 2017;389:1550-7.[PubMed Abstract] -
- 21.Pourang A, Fung MA, Tartar D, Brassard A. Condyloma lata in secondary syphilis. JAAD Case Rep. 2021;10:18-21.[PubMed Abstract] -
- 22.Marx GE, Dhanireddy S, Marrazzo JM, et al. Variations in clinical presentation of ocular syphilis: case series reported from a growing epidemic in the United States. Sex Transm Dis. 2016;43:519-23.[PubMed Abstract] -
- 23.Woolston SL, Dhanireddy S, Marrazzo J. Ocular syphilis: a clinical review. Curr Infect Dis Rep. 2016;18:36.[PubMed Abstract] -
- 24.Ramchandani MS, Litvack JR, Marra CM. Otosyphilis: A Review of the Literature. Sex Transm Dis. 2020;47:296-300.[PubMed Abstract] -
- 25.Theeuwen H, Whipple M, Litvack JR. Otosyphilis: Resurgence of an Old Disease. Laryngoscope. 2019;129:1680-4.[PubMed Abstract] -
- 26.Papp JR, Park IU, Fakile Y, Pereira L, Pillay A, Bolan GA. CDC Laboratory Recommendations for Syphilis Testing, United States, 2024. MMWR Recomm Rep. 2024;73:1-32.[PubMed Abstract] -
- 27.Satyaputra F, Hendry S, Braddick M, Sivabalan P, Norton R. The Laboratory Diagnosis of Syphilis. J Clin Microbiol. 2021;59:e0010021.[PubMed Abstract] -
- 28.National Syphilis and Congenital Syphilis Syndemic Federal Task Force. Considerations for the Implementation of Point of Care (POC) Tests for Syphilis. June 2024[HHS] -
- 29.Manikowska-Lesińska W, Linda B, Zajac W. Specificity of the FTA-ABS and TPHA tests during pregnancy. Br J Vener Dis. 1978;54:295-8.[PubMed Abstract] -
- 30.Henrich TJ, Yawetz S. Impact of age, gender, and pregnancy on syphilis screening using the Captia Syphilis-G assay. Sex Transm Dis. 201138:1126-30.[PubMed Abstract] -
- 31.Henrich TJ, Yawetz S. Impact of age, gender, and pregnancy on syphilis screening using the Captia Syphilis-G assay. Sex Transm Dis. 2011;38:1126-30.[PubMed Abstract] -
- 32.American College of Obstetricians and Gynecologists (ACOG). Screening for Syphilis in Pregnancy Practice Advisory. April 2024.[ACOG] -
- 33.Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021. Detection of STIs in special populations: pregnant women. MMWR Recomm Rep. 2021;70(No. RR-4):1-187.
- 34.Silverstein M, Wong JB, Davis EM, et al. Screening for Syphilis Infection During Pregnancy: US Preventive Services Task Force Reaffirmation Recommendation Statement. JAMA. 2025 May 13. Online ahead of print.[PubMed Abstract] -
- 35.Centers for Disease Control and Prevention (CDC). STI Statistics. County-level Syphilis Data
- 36.Rac MWF, Stafford IA, Eppes CS. Congenital syphilis: A contemporary update on an ancient disease. Prenat Diagn. 2020;40:1703-1714.[PubMed Abstract] -
- 37.Rac MW, Bryant SN, McIntire DD, et al. Progression of ultrasound findings of fetal syphilis after maternal treatment. Am J Obstet Gynecol. 2014;211:426.e1-6.[PubMed Abstract] -
- 38.Hira SK, Bhat GJ, Patel JB, et al. Early congenital syphilis: clinico-radiologic features in 202 patients. Sex Transm Dis. 1985;12:177-83.[PubMed Abstract] -
- 39.Rolfs RT. Treatment of syphilis, 1993. Clin Infect Dis. 1995;20 Suppl 1:S23-38.[PubMed Abstract] -
- 40.Alexander JM, Sheffield JS, Sanchez PJ, Mayfield J, Wendel GD Jr. Efficacy of treatment for syphilis in pregnancy. Obstet Gynecol. 1999;93:5-8.[PubMed Abstract] -
- 41.Zhu L, Qin M, Du L, Xie RH, Wong T, Wen SW. Maternal and congenital syphilis in Shanghai, China, 2002 to 2006. Int J Infect Dis. 2010;14 Suppl 3:e45-8.[PubMed Abstract] -
- 42.Wendel GD Jr, Sheffield JS, Hollier LM, Hill JB, Ramsey PS, Sánchez PJ. Treatment of syphilis in pregnancy and prevention of congenital syphilis. Clin Infect Dis. 2002;35:S200-9.[PubMed Abstract] -
- 43.Hawkes S, Matin N, Broutet N, Low N. Effectiveness of interventions to improve screening for syphilis in pregnancy: a systematic review and meta-analysis. Lancet Infect Dis. 2011;11:684-91.[PubMed Abstract] -
- 44.Nathan L, Bawdon RE, Sidawi JE, Stettler RW, McIntire DM, Wendel GD Jr. Penicillin levels following the administration of benzathine penicillin G in pregnancy. Obstet Gynecol. 1993;82:338-42.[PubMed Abstract] -
- 45.Eppes CS, Stafford I, Rac M. Syphilis in pregnancy: an ongoing public health threat. Am J Obstet Gynecol. 2022;227:822-38.[PubMed Abstract] -
- 46.Wendel GD Jr, Stark BJ, Jamison RB, Molina RD, Sullivan TJ. Penicillin allergy and desensitization in serious infections during pregnancy. N Engl J Med. 1985;312:1229-32.[PubMed Abstract] -
- 47.Ziaya PR, Hankins GD, Gilstrap LC 3rd, Halsey AB. Intravenous penicillin desensitization and treatment during pregnancy. JAMA. 1986;256:2561-2.[PubMed Abstract] -
- 48.Brown ST. Adverse reactions in syphilis therapy. J Am Vener Dis Assoc. 1976;3:172-6.[PubMed Abstract] -
- 49.Dhaliwal A, Lopez AA, Bullard J, Poliquin V. Local incidence of Jarisch-Herxheimer reaction in pregnancy following penicillin treatment for syphilis: A case series. J Assoc Med Microbiol Infect Dis Can. 2021;6:319-24.[PubMed Abstract] -
- 50.Mori H, Shibata E, Kondo E, Sasaki N, Sawada Y, Yoshino K. The incidence of Jarisch-Herxheimer reactions and associated risk factors in pregnant women and nonpregnant women: A retrospective chart review at a university hospital in Japan. J Obstet Gynaecol Res. 2023;49:1435-42.[PubMed Abstract] -
- 51.Hollier LM, Harstad TW, Sanchez PJ, Twickler DM, Wendel GD Jr. Fetal syphilis: clinical and laboratory characteristics. Obstet Gynecol. 2001;97:947-53.[PubMed Abstract] -
- 52.Ramsey PS. Editorial commentary: post-syphilotherapy titers in pregnancy. Clin Infect Dis. 2015;60:691-2.[PubMed Abstract] -
- 53.Macumber S, Singh AE, Gratrix J, et al. Retrospective Cohort Study of the Incidence and Outcomes of Jarisch-Herxheimer Reactions After Treatment of Infectious Syphilis in Late Pregnancy. Sex Transm Dis. 2022;49:e107-e109.[PubMed Abstract] -
- 54.Rac MW, Bryant SN, Cantey JB, McIntire DD, Wendel GD Jr, Sheffield JS. Maternal titers after adequate syphilotherapy during pregnancy. Clin Infect Dis. 2015;60:686-90.[PubMed Abstract] -
- 55.Ghanem KG, Hook EW 3rd. The terms "serofast" and "serological nonresponse" in the modern syphilis era. Sex Transm Dis. 2021;48:451-2.[PubMed Abstract] -
- 56.Rathbun KC. Congenital syphilis. Sex Transm Dis. 1983;10:93-9.[PubMed Abstract] -
- 59.Lafond RE, Lukehart SA. Biological basis for syphilis. Clin Microbiol Rev. 2006;19:29-49.[PubMed Abstract] -
- 60.Cremin BJ, Fisher RM. The lesions of congenital syphilis. Br J Radiol. 1970;43:333-41.[PubMed Abstract] -
- 61.Newton J, Silence C, Boetes J, Cohen BA. Mucocutaneous manifestations of congenital syphilis in the neonate: A review of a surging disease. Pediatr Dermatol. 2023;40:238-41.[PubMed Abstract] -
- 62.Fanella S, Bitnun A, Barton M, Sauvé L. Diagnosis and management of congenital syphilis: Avoiding missed opportunities. Paediatr Child Health. 2024;29:463-79.[PubMed Abstract] -
- 63.Sankaran D, Partridge E, Lakshminrusimha S. Congenital Syphilis-An Illustrative Review. Children (Basel). 2023;10:1310.[PubMed Abstract] -
- 64.Fiumara NJ, Lessell S. Manifestations of late congenital syphilis. An analysis of 271 patients. Arch Dermatol. 1970;102:78-83.[PubMed Abstract] -
- 65.Grimprel E, Sanchez PJ, Wendel GD, et al. Use of polymerase chain reaction and rabbit infectivity testing to detect Treponema pallidum in amniotic fluid, fetal and neonatal sera, and cerebrospinal fluid. J Clin Microbiol. 1991;29:1711-8.[PubMed Abstract] -
- 66.Sánchez PJ, Wendel GD Jr, Grimprel E, et al. Evaluation of molecular methodologies and rabbit infectivity testing for the diagnosis of congenital syphilis and neonatal central nervous system invasion by Treponema pallidum. J Infect Dis. 1993;167:148-57.[PubMed Abstract] -
- 67.Sheffield JS, Sánchez PJ, Wendel GD Jr, et al. Placental histopathology of congenital syphilis. Obstet Gynecol. 2002;100:126-33.[PubMed Abstract] -
- 68.Dunn RA, Zenker PN. Why radiographs are useful in evaluation of neonates suspected of having congenital syphilis. Radiology. 1992;182:639-40.[PubMed Abstract] -
- 69.Rasool MN, Govender S. The skeletal manifestations of congenital syphilis. A review of 197 cases. J Bone Joint Surg Br. 1989;71:752-5.[PubMed Abstract] -
Additional References
- Ahmed KA, Fox SJ, Frigas E, Park MA. Clinical outcome in the use of cephalosporins in pediatric patients with a history of penicillin allergy. Int Arch Allergy Immunol. 2012;158:405-10.[PubMed Abstract] -
- Aires Figueiredo L, Botelho Brito T, Labrusco M, Brigham Figueiredo M, Lopo Tuna M. A Rare But Pathognomonic Sign of Congenital Syphilis. J Pediatr. 2023;262:113622.[PubMed Abstract] -
- Azqul MM, Griner SB, Pinto CN. Congenital Syphilis in the US: A Narrative Review. Sex Transm Dis. 2025;52:211-2.[PubMed Abstract] -
- Banks DB, Flores JM, Paredes JL, Parzen-Johnson SL. Evaluation and Treatment of Congenital Syphilis: A National Survey of US Pediatric Specialists. J Clin Med. 2024;13:6280.[PubMed Abstract] -
- Berkowitz K, Baxi L, Fox HE. False-negative syphilis screening: the prozone phenomenon, nonimmune hydrops, and diagnosis of syphilis during pregnancy. Am J Obstet Gynecol. 1990;163:975-7.[PubMed Abstract] -
- Cross JB, McCain JR, Heyman A. The use of crystalline penicillin G in the treatment of syphilis in pregnancy. Am J Obstet Gynecol. 1949;57:461-5.[PubMed Abstract] -
- Curry SJ, Krist AH, Owens DK, et al. Screening for Syphilis Infection in Pregnant Women: US Preventive Services Task Force Reaffirmation Recommendation Statement. JAMA. 2018;320:911-7.[PubMed Abstract] -
- Desravines N, Waldron J, Venkatesh KK, Kwan M, Boggess KA. Outpatient Penicillin Allergy Testing in Pregnant Women Who Report an Allergy. Obstet Gynecol. 2021;137:56-61.[PubMed Abstract] -
- Donders GG, Desmyter J, Hooft P, Dewet GH. Apparent failure of one injection of benzathine penicillin G for syphilis during pregnancy in human immunodeficiency virus-seronegative African women. Sex Transm Dis. 1997;24:94-101.[PubMed Abstract] -
- Flores JM, Kasal N, Montag C, et al. Factors Related to the Rise of Congenital Syphilis From the Perspectives of Prenatal Providers and Birthing Parents in Chicago, IL, USA. Open Forum Infect Dis. 2024;11:ofae595.[PubMed Abstract] -
- Fukuda A, Katz AR, Park IU, et al. Congenital Syphilis: A Case Report Demonstrating Missed Opportunities for Screening and Inadequate Treatment Despite Multiple Health Care Encounters During Pregnancy. Sex Transm Dis. 2021;48:e124-e125.[PubMed Abstract] -
- Galan HL, Montalvo JF, Deaver J. Retrospective analysis of the serologic response to the treatment of syphilis during pregnancy. Infect Dis Obstet Gynecol. 1997;5:23-8.[PubMed Abstract] -
- Ghanem KG. Management of Adult Syphilis: Key Questions to Inform the 2015 Centers for Disease Control and Prevention Sexually Transmitted Diseases Treatment Guidelines. Clin Infect Dis. 2015;61 Suppl 8:S818-36.[PubMed Abstract] -
- Kidd S, Bowen VB, Torrone EA, Bolan G. Use of National Syphilis Surveillance Data to Develop a Congenital Syphilis Prevention Cascade and Estimate the Number of Potential Congenital Syphilis Cases Averted. Sex Transm Dis. 2018;45:S23-S28.[PubMed Abstract] -
- Klein VR, Cox SM, Mitchell MD, Wendel GD Jr. The Jarisch-Herxheimer reaction complicating syphilotherapy in pregnancy. Obstet Gynecol. 1990;75:375-80.[PubMed Abstract] -
- Machefsky AM, Loosier PS, Cramer R, et al. A New Call to Action to Combat an Old Nemesis: Addressing Rising Congenital Syphilis Rates in the United States. J Womens Health (Larchmt). 2021;30:920-6.[PubMed Abstract] -
- Myles TD, Elam G, Park-Hwang E, Nguyen T. The Jarisch-Herxheimer reaction and fetal monitoring changes in pregnant women treated for syphilis. Obstet Gynecol. 1998;92:859-64.[PubMed Abstract] -
- Peterman TA, Newman DR, Davis D, Su JR. Do women with persistently negative nontreponemal test results transmit syphilis during pregnancy? Sex Transm Dis. 2013;40:311-5.[PubMed Abstract] -
- Qin J, Yang T, Xiao S, Tan H, Feng T, Fu H. Reported estimates of adverse pregnancy outcomes among women with and without syphilis: a systematic review and meta-analysis. PLoS One. 2014;9:e102203.[PubMed Abstract] -
- Saloojee H, Velaphi S, Goga Y, Afadapa N, Steen R, Lincetto O. The prevention and management of congenital syphilis: an overview and recommendations. Bull World Health Organ. 2004;82:424-30.[PubMed Abstract] -
- Seña AC, Wolff M, Martin DH, et al. Predictors of serological cure and Serofast State after treatment in HIV-negative persons with early syphilis. Clin Infect Dis. 2011;53:1092-9.[PubMed Abstract] -
- Seña AC, Zhang XH, Li T, et al. A systematic review of syphilis serological treatment outcomes in HIV-infected and HIV-uninfected persons: rethinking the significance of serological non-responsiveness and the serofast state after therapy. BMC Infect Dis. 2015;15:479.[PubMed Abstract] -
- Sheffield JS, Sánchez PJ, Morris G, et al. Congenital syphilis after maternal treatment for syphilis during pregnancy. Am J Obstet Gynecol. 2002;186:569-73.[PubMed Abstract] -
- Slutsker JS, Hennessy RR, Schillinger JA. Factors Contributing to Congenital Syphilis Cases - New York City, 2010-2016. MMWR Morb Mortal Wkly Rep. 2018 Oct 5;67:1088-1093.[PubMed Abstract] -
- Slutsker JS, Hennessy RR, Schillinger JA. Factors Contributing to Congenital Syphilis Cases - New York City, 2010-2016. MMWR Morb Mortal Wkly Rep. 2018;67:1088-93.[PubMed Abstract] -
- Thornton C, Chaisson LH, Bleasdale SC. Characteristics of Pregnant Women With Syphilis and Factors Associated With Congenital Syphilis at a Chicago Hospital. Open Forum Infect Dis. 2022;9:ofac169.[PubMed Abstract] -
- Trivedi S, Williams C, Torrone E, Kidd S. National Trends and Reported Risk Factors Among Pregnant Women With Syphilis in the United States, 2012-2016. Obstet Gynecol. 2019;133:27-32.[PubMed Abstract] -
- Tuddenham S, Ghanem KG. Management of Adult Syphilis: Key Questions to Inform the 2021 Centers for Disease Control and Prevention Sexually Transmitted Infections Treatment Guidelines. Clin Infect Dis. 2022;74:S127-S133.[PubMed Abstract] -
- U.S. Food and Drug Administration. Doxycycline use by pregnant and lactating women. Food and Drug Administration, 2017[US FDA] -
Figures
 Figure 1. Point of Intervention for Prevention of Congenital SyphilisIllustration: David H. Spach, MD
Figure 1. Point of Intervention for Prevention of Congenital SyphilisIllustration: David H. Spach, MD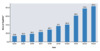 Figure 2 (Image Series). Syphilis in Women of Child-Bearing Age in the United StatesSource: Centers for Disease Control and Prevention. Sexually Transmitted Infections Surveillance, 2023. Atlanta: U.S. Department of Health and Human Services; 2024.
Figure 2 (Image Series). Syphilis in Women of Child-Bearing Age in the United StatesSource: Centers for Disease Control and Prevention. Sexually Transmitted Infections Surveillance, 2023. Atlanta: U.S. Department of Health and Human Services; 2024. Figure 3 (Image Series). Congenital Syphilis in the United StatesSource: Centers for Disease Control and Prevention. Sexually Transmitted Infections Surveillance, 2023. Atlanta: U.S. Department of Health and Human Services; 2024.
Figure 3 (Image Series). Congenital Syphilis in the United StatesSource: Centers for Disease Control and Prevention. Sexually Transmitted Infections Surveillance, 2023. Atlanta: U.S. Department of Health and Human Services; 2024.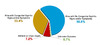 Figure 4. Congenital Syphilis — Reported Cases by Vital Status and Clinical Signs and Symptoms* of Infection, United States, 2019–2023*Neonates with signs and/or symptoms of congenital syphilis have documentation of ≥1 of the following: long bone changes, snuffles, condylomata lata, syphilitic skin rash, pseudoparalysis, hepatosplenomegaly, edema, jaundice due to syphilitic hepatitis, reactive CSF-VDRL, elevated CSF WBC or protein values, or evidence of direct detection of T. pallidum.Source: Centers for Disease Control and Prevention. Sexually Transmitted Infections Surveillance, 2023. Atlanta: U.S. Department of Health and Human Services; 2024.
Figure 4. Congenital Syphilis — Reported Cases by Vital Status and Clinical Signs and Symptoms* of Infection, United States, 2019–2023*Neonates with signs and/or symptoms of congenital syphilis have documentation of ≥1 of the following: long bone changes, snuffles, condylomata lata, syphilitic skin rash, pseudoparalysis, hepatosplenomegaly, edema, jaundice due to syphilitic hepatitis, reactive CSF-VDRL, elevated CSF WBC or protein values, or evidence of direct detection of T. pallidum.Source: Centers for Disease Control and Prevention. Sexually Transmitted Infections Surveillance, 2023. Atlanta: U.S. Department of Health and Human Services; 2024. Figure 5. Risk of Vertical Transmission Based on Maternal Syphilis StageEarly latent syphilis is defined as maternal infection of less than a year’s duration and late latent infection greater than a year’s duration.Source: Medoro AK, Sánchez PJ. Syphilis in Neonates and Infants. Clin Perinatol. 2021;48:293-309.
Figure 5. Risk of Vertical Transmission Based on Maternal Syphilis StageEarly latent syphilis is defined as maternal infection of less than a year’s duration and late latent infection greater than a year’s duration.Source: Medoro AK, Sánchez PJ. Syphilis in Neonates and Infants. Clin Perinatol. 2021;48:293-309. Figure 6. Syphilis StagesAfter initial exposure to Treponema pallidum, the incubation period ranges from 10–90 days.Illustration: David H. Spach, MD
Figure 6. Syphilis StagesAfter initial exposure to Treponema pallidum, the incubation period ranges from 10–90 days.Illustration: David H. Spach, MD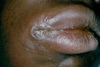 Figure 7 (Image Series). Primary SyphilisPhotograph Credit: Centers for Disease Control and Prevention Public Health Image Library (Robert E. Sumpter, 1967).
Figure 7 (Image Series). Primary SyphilisPhotograph Credit: Centers for Disease Control and Prevention Public Health Image Library (Robert E. Sumpter, 1967).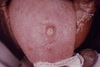 Figure 7B. Primary Syphilis (Chancre) in Woman on TonguePhotograph Credit: Centers for Disease Control and Prevention Public Health Image Library (Robert E. Sumpter, 1967).
Figure 7B. Primary Syphilis (Chancre) in Woman on TonguePhotograph Credit: Centers for Disease Control and Prevention Public Health Image Library (Robert E. Sumpter, 1967). Figure 8 (Image Series). Manifestations of Secondary Syphilis in WomenPhotograph credit: Negusse Ocbamichael, PA; Public Health—Seattle & King County Sexual Health Clinic
Figure 8 (Image Series). Manifestations of Secondary Syphilis in WomenPhotograph credit: Negusse Ocbamichael, PA; Public Health—Seattle & King County Sexual Health Clinic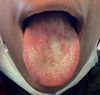 Figure 8B. Oral Mucous Patches in a Woman with Secondary SyphilisPhotograph credit: Negusse Ocbamichael, PA; Public Health—Seattle & King County Sexual Health Clinic
Figure 8B. Oral Mucous Patches in a Woman with Secondary SyphilisPhotograph credit: Negusse Ocbamichael, PA; Public Health—Seattle & King County Sexual Health Clinic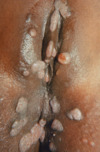 Figure 8C. Condylomata Lata in a Woman with Secondary SyphilisPhotograph Credit: Centers for Disease Control and Prevention Public Health Image Library (Joyce Ayers, 1968).
Figure 8C. Condylomata Lata in a Woman with Secondary SyphilisPhotograph Credit: Centers for Disease Control and Prevention Public Health Image Library (Joyce Ayers, 1968).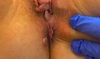 Figure 8D. Condylomata Lata in a Woman with Secondary SyphilisPhotograph credit: Negusse Ocbamichael, PA; Public Health—Seattle & King County Sexual Health Clinic
Figure 8D. Condylomata Lata in a Woman with Secondary SyphilisPhotograph credit: Negusse Ocbamichael, PA; Public Health—Seattle & King County Sexual Health Clinic Figure 9 (Image Series). Syphilis Screening Algorithms for Pregnant Women*This denotes laboratory-based syphilis serologic tests.
Figure 9 (Image Series). Syphilis Screening Algorithms for Pregnant Women*This denotes laboratory-based syphilis serologic tests.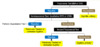 Figure 9B. Initial Screening with Treponemal Test (Reverse Screening Algorithm)Source: Papp JR, Park IU, Fakile Y, Pereira L, Pillay A, Bolan GA. CDC Laboratory Recommendations for Syphilis Testing, United States, 2024. MMWR Recomm Rep. 2024;73:1-32.
Figure 9B. Initial Screening with Treponemal Test (Reverse Screening Algorithm)Source: Papp JR, Park IU, Fakile Y, Pereira L, Pillay A, Bolan GA. CDC Laboratory Recommendations for Syphilis Testing, United States, 2024. MMWR Recomm Rep. 2024;73:1-32.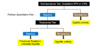 Figure 9C. Initial Screening with Nontreponemal Test (Traditional Screening Algorithm)Source: Papp JR, Park IU, Fakile Y, Pereira L, Pillay A, Bolan GA. CDC Laboratory Recommendations for Syphilis Testing, United States, 2024. MMWR Recomm Rep. 2024;73:1-32.
Figure 9C. Initial Screening with Nontreponemal Test (Traditional Screening Algorithm)Source: Papp JR, Park IU, Fakile Y, Pereira L, Pillay A, Bolan GA. CDC Laboratory Recommendations for Syphilis Testing, United States, 2024. MMWR Recomm Rep. 2024;73:1-32. Figure 10 (Image Series). Timeline to Resolution of Abnormal Fetal Ultrasound FindingsSource: Rac MW, Bryant SN, McIntire DD, et al. Progression of ultrasound findings of fetal syphilis after maternal treatment. Am J Obstet Gynecol. 2014;211:426.e1-6. Reproduced with permission from Elsevier. American Journal of Obstetrics & Gynecology.
Figure 10 (Image Series). Timeline to Resolution of Abnormal Fetal Ultrasound FindingsSource: Rac MW, Bryant SN, McIntire DD, et al. Progression of ultrasound findings of fetal syphilis after maternal treatment. Am J Obstet Gynecol. 2014;211:426.e1-6. Reproduced with permission from Elsevier. American Journal of Obstetrics & Gynecology. Figure 11. Treatment of Syphilis in PregnancyThis figure is based on recommendations in the 2021 Sexually Transmitted Infections Treatment GuidelinesIllustration: David H. Spach, MD
Figure 11. Treatment of Syphilis in PregnancyThis figure is based on recommendations in the 2021 Sexually Transmitted Infections Treatment GuidelinesIllustration: David H. Spach, MD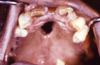 Figure 12 (Image Series). Oral Manifestations with Congenital SyphilisThis photograph shows an intraoral view of a perforation in the hard palate caused by congenital syphilis.Photograph credit: Centers for Disease Control and Prevention Public Health Image Library (CDC. Robert E. Sumpter, 1967).
Figure 12 (Image Series). Oral Manifestations with Congenital SyphilisThis photograph shows an intraoral view of a perforation in the hard palate caused by congenital syphilis.Photograph credit: Centers for Disease Control and Prevention Public Health Image Library (CDC. Robert E. Sumpter, 1967).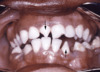 Figure 12B. Congenital Syphilis—Hutchinson's TeethThis photograph demonstrates the triangular-shaped deformity of an upper central incisor (top arrow) and a lower lateral incisor (lower arrow) dentition within the oral cavity of a person with a history of congenital syphilis. These dental abnormalities are known as Hutchinson incisors.Photograph credit: Centers for Disease Control and Prevention Public Health Image Library (CDC Robert E. Sumpter, 1967).
Figure 12B. Congenital Syphilis—Hutchinson's TeethThis photograph demonstrates the triangular-shaped deformity of an upper central incisor (top arrow) and a lower lateral incisor (lower arrow) dentition within the oral cavity of a person with a history of congenital syphilis. These dental abnormalities are known as Hutchinson incisors.Photograph credit: Centers for Disease Control and Prevention Public Health Image Library (CDC Robert E. Sumpter, 1967). Figure 13. Treatment Scenarios Based on Likelihood of Congenital SyphilisThe four categories shown reflect the likelihood of a diagnosis of congenital syphilis in the neonate. These categories are based on maternal syphilis history and evaluation of the neonate. These scenarios only include neonates born to women who have reactive nontreponemal and treponemal serologic tests for syphilis during pregnancy (e.g., RPR reactive, TP-PA reactive or EIA reactive, RPR reactive) and have a reactive nontreponemal test at delivery (e.g., RPR reactive).Illustration: David H. Spach, MD
Figure 13. Treatment Scenarios Based on Likelihood of Congenital SyphilisThe four categories shown reflect the likelihood of a diagnosis of congenital syphilis in the neonate. These categories are based on maternal syphilis history and evaluation of the neonate. These scenarios only include neonates born to women who have reactive nontreponemal and treponemal serologic tests for syphilis during pregnancy (e.g., RPR reactive, TP-PA reactive or EIA reactive, RPR reactive) and have a reactive nontreponemal test at delivery (e.g., RPR reactive).Illustration: David H. Spach, MDTables
Table 1. 2021 STI Treatment Guidelines: Syphilis During PregnancyTreatment of Primary and Secondary Syphilis During PregnancyPenicillin G is the only known effective antimicrobial for treating fetal infection and preventing congenital syphilis.Recommended RegimenBenzathine penicillin G2.4 million units IM in a single doseBenzathine penicillin G
Tradename:Bicillin-LANote: Some experts recommend giving a second dose of intramuscular benzathine penicillin G 2.4 million units 1 week after the initial penicillin dose, especially when syphilis is treated after 20 weeks of pregnancy.Source: Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021. Syphilis. MMWR Recomm Rep. 2021;70(No. RR-4):1-187. [2021 STI Treatment Guidelines]Table 2. 2021 STI Treatment Guidelines: Syphilis During PregnancyTreatment of Latent Syphilis During PregnancyRecommended Regimen for Early Latent SyphilisBenzathine penicillin G2.4 million units IM in a single doseBenzathine penicillin G
Tradename:Bicillin-LANote: Some experts recommend giving a second dose of intramuscular benzathine penicillin G 2.4 million units 1 week after the initial penicillin dose, especially when syphilis is treated after 20 weeks of pregnancy.Recommended Regimen for Late Latent Syphilis (and latent Syphili of Unknown Duration)Benzathine penicillin G7.2 million units total, administered as 3 doses of 2.4 million units IM at 1-week intervalsBenzathine penicillin G
Tradename:Bicillin-LANote: Any benzathine penicillin dose that is not given within 9 days of the prior dose is considered an unacceptable gap in treatment, and the entire 3-dose series must be started over.Source: Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021. Syphilis. MMWR Recomm Rep. 2021;70(No. RR-4):1-187. [2021 STI Treatment Guidelines]Table 3. 2021 STI Treatment Guidelines: Syphilis During PregnancyTreatment of Neurosyphilis, Ocular Syphilis, or Otosyphilis During PregnancyNote: procaine penicillin G is no longer available for use and therefore is not included in this table.Recommended RegimenAqueous crystalline penicillin G18–24 million units per day, administered as 3–4 million units IV every 4 hours or continuous infusion, for 10–14 daysAqueous crystalline penicillin G
Tradename:PfizerpenThe duration of the recommended treatment for neurosyphilis is shorter than the total duration of treatment used for latent syphilis. Therefore, benzathine penicillin G, 2.4 million units IM once per week for up to 3 weeks, can be considered after completion of the neurosyphilis treatment to provide a total duration of therapy comparable to the treatment of latent syphilis.Source: Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021. Syphilis. MMWR Recomm Rep. 2021;70(No. RR-4):1-187. [2021 STI Treatment Guidelines]Table 4. Success of Maternal Treatment of Syphilis in Preventing Congenital Syphilis, by Maternal Syphilis Stage
Maternal Syphilis Stage Success* / Total Treated Percentage Success* Primary 27/27 100% Secondary 71/75 94.7% Early Latent 100/102 98.0% Late Latent 136/136 100% All Stages 334/340 98.2% *Success defined as preventing congenital syphilis
Source:- Alexander JM, Sheffield JS, Sanchez PJ, Mayfield J, Wendel GD Jr. Efficacy of treatment for syphilis in pregnancy. Obstet Gynecol. 1999;93:5-8. [PubMed Abstract]
Table 5. Success of Maternal Treatment of Syphilis in Preventing Congenital Syphilis, by Gestational Age
Gestational Age Success* / Total Treated Percentage Success* ≤20 weeks 152/153 99.4% 21-25 weeks 51/51 100% 26-30 weeks 58/59 98.3% 31-35 weeks 44/46 95.6% 36-40 weeks 26/28 92.9% 41-42 weeks 3/3 100% All Gestational Ages 334/340 98.2% *Success defined as preventing congenital syphilis
Source:- Alexander JM, Sheffield JS, Sanchez PJ, Mayfield J, Wendel GD Jr. Efficacy of treatment for syphilis in pregnancy. Obstet Gynecol. 1999;93:5-8. [PubMed Abstract]
Table 6. 2021 STI Treatment Guidelines: Congenital SyphilisTreatment of Confirmed or Highly Probable Congenital SyphilisProcaine penicillin G is no longer available in the United States and therefore is not included in this table.Recommended for Treatment of Confirmed or Highly Probable Congenital SyphilisAqueous crystalline penicillin G100,000–150,000 units/kg body weight/day, administered as 50,000 units/kg body weight/dose IV every 12 hours for doses given during the first 7 days of life and every 8 hours thereafter for a total of 10 daysAqueous crystalline penicillin G
Tradename:PfizerpenNote: If more than 1 day of penicillin therapy is missed, the entire course should be restarted.Source: Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021. Syphilis. MMWR Recomm Rep. 2021;70(No. RR-4):1-187. [2021 STI Treatment Guidelines]Table 7. 2021 STI Treatment Guidelines: Congenital SyphilisTreatment of Possible Congenital SyphilisProcaine penicillin G is no longer available in the United States and therefore is not included in this table.Recommended for Treatment of Possible Congenital SyphilisAqueous crystalline penicillin G100,000–150,000 units/kg body weight/day, administered as 50,000 units/kg body weight/dose IV every 12 hours during the first 7 days of life and every 8 hours thereafter for a total of 10 daysAqueous crystalline penicillin G
Tradename:PfizerpenNote: If more than 1 day of penicillin therapy is missed, the entire course should be restarted.Recommended for Treatment of Possible Congenital SyphilisBenzathine penicillin G50,000 units/kg body weight/dose IM in a single doseBenzathine penicillin G
Tradename:Bicillin-LANote: The single-dose benzathine penicillin G intramuscular dose should only be considered if the recommended evaluation has been completed, all results of the evaluation are normal, and follow-up is certain.Source: Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021. Syphilis. MMWR Recomm Rep. 2021;70(No. RR-4):1-187. [2021 STI Treatment Guidelines]Table 8. 2021 STI Treatment Guidelines: Congenital SyphilisTreatment When Congenital Syphilis Less LikelyRecommended for Treatment When Congenital Syphilis Less LikelyBenzathine penicillin G50,000 units/kg body weight/dose IM in a single doseBenzathine penicillin G
Tradename:Bicillin-LAAnother approach involves not treating the newborn if follow-up is certain but providing close serologic follow-up every 2–3 months for 6 months for infants whose mothers' nontreponemal titers decreased at least fourfold after therapy for early syphilis or remained stable for low- titer, latent syphilis (e.g., VDRL <1:2 orSource: Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021. Syphilis. MMWR Recomm Rep. 2021;70(No. RR-4):1-187. [2021 STI Treatment Guidelines]Table 9. 2021 STI Treatment Guidelines: SyphilisTreatment of Congenital Syphilis Among Infants and ChildrenInfants and children aged ≥1 month who receive a syphilis diagnosis should have birth and maternal medical records reviewed to assess whether they have congenital or acquired syphilis.Recommended RegimenAqueous crystalline penicillin G200,000–300,000 units/kg body weight/day by IV, administered as 50,000 units/kg body weight every 4–6 hours for 10 daysAqueous crystalline penicillin G
Tradename:PfizerpenIf the infant or child has no clinical manifestations of congenital syphilis and the evaluation (including the CSF examination) is normal, treatment with up to 3 weekly doses of benzathine penicillin G 50,000 units/kg body weight IM can be considered. A single dose of benzathine penicillin G 50,000 units/kg body weight IM up to the adult dose of 2.4 million units in a single dose can be considered after the 10-day course of IV aqueous penicillin G to provide more comparable duration for treatment in those wInfants and children aged ≥1 month with primary or secondary syphilis should be managed by a pediatric infectious disease specialist and evaluated for sexual abuse (e.g. through consultation with child-protection services)Source: Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021. Syphilis. MMWR Recomm Rep. 2021;70(No. RR-4):1-187. [2021 STI Treatment Guidelines]Share by e-mail
Check
-On-
Learning
QuestionsThe Check-on-Learning Questions are short and topic related. They are meant to help you stay on track throughout each lesson and check your understanding of key concepts.You must be signed in to customize your interaction with these questions.
Since you've received 80% or better on this quiz, you may claim continuing education credit.
You seem to have a popup blocker enabled. If you want to skip this dialog please Always allow popup windows for the online course.
Current Version: nstdc-monorepo-47246f17-2026-01-09-011457Become a New UserAccount Registration Benefits:
- Track your progress on the lessons
- Earn free CNE/CME/CE
- Earn Certificates of Completion
- Access to other free IDEA curricula
Create a free account to get started
- 0%Lesson 2


























